Infertility: The science, the myths and the solutions
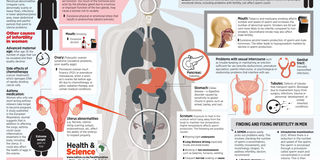
The science of fertility and why some men and women have difficulties with conception. GRAPHIC| MICHAEL MOSOTA
A woman’s fertility starts to decline steadily from age 20 to 30, with a rapid decline after she hits 35. Between age 20 to 30, the probability of conceiving declines from 30 to 25 per cent every month.
By age 40, the probability is less than five per cent, and negligible after age 45.
This is because a woman is born with all the eggs she will ever have, starting with six to seven million eggs as a foetus. This is in contrast with men whose ability to produce sperm is limitless, with average sperm production going up to 100 million per day.
By the time a woman is born, the number of eggs has declined to one to two million. By puberty when the reproductive phase kicks off, the number is down to 300,000. About 450 eggs will be ovulated during menstrual cycles, with the others undergoing natural cell death. By menopause the eggs have declined to 1,000.
Male fertility also declines with age but not as dramatically. Studies done in North America have shown that fertility after age 40 declines by 30 per cent.
While the sperm count does not decrease dramatically with age, the movement of sperms declines nominally (0.8 per cent per year) while the shape deteriorates by 0.9 per cent every year.
Decline in sexual frequency with age, due to sexual dysfunction, also affects fertility. There is also a higher rate of DNA fragmentation, which decreases the genetic quality of the sperm with age.
However, some men think that ability to have sex and ejaculate is proof of fertility, while others think that as long as no one in their family had a problem, they can’t be suffering from infertility.
They couldn’t be more off the mark!
If things are working as they should, a woman’s body releases an egg from one of her ovaries (ovulation) every month/menstrual cycle. It moves down the fallopian tube towards the uterus, and if it meets a sperm along the way, fertilisation takes place. The fertilised egg continues with its journey towards the uterus, where it attaches itself (implantation) to start a pregnancy.
After ovulation, the egg lasts 12 to 24 hours, after which it dies. Sperms, on the other hand, remain in the body for about five days, waiting for their chance meeting with the egg.
Therefore, unprotected sex a few days before ovulation or during ovulation, raises chances for the egg and sperm to meet.
However, some couples struggle, taking longer to conceive, despite a full year of regular unprotected sex. The World Health Organisation says that in 38 per cent of the cases, infertility can be attributed to the woman, in 30 to 40 per cent of the cases, the man, 27 per cent of the time to both, and 15 per cent of the time to neither.
One in six couples are afflicted and might have to turn to assisted reproductive technologies such as in vitro fertilisation, with all the sacrifices, financial constraints and physical and emotional upheaval that may come with it. Both men and women may take this difficulty to mean their masculinity/femininity is diminished, leading to mental distress.
It can’t be emphasised enough that men do contribute to infertility, even though infertility research has focused on women.
As such, intracytoplasmic sperm injection (ICSI)—where the sperm is placed into the egg rather than next to it and IVF do not treat the male problem, but instead bypass it.
***
Syndrome that plagues many women who are having difficulties conceiving
BY EUNICE KILONZO
Polycystic ovarian syndrome (PCOS) is a common hormonal problem that affects the ovaries. Dr Jane Machira, a fertility expert based in Nairobi, says that for every 10 women seeking help for fertility problems, three to four have PCOS.
It is characterised by many small cysts (fluid-filled sacs) on one or both ovaries, higher androgen (male hormones) levels, and irregular menstrual cycle. The cysts are not cancerous. Along with infertility, women with PCOS are at higher risk for miscarriage and pregnancy complications, as well as obesity, type 2 diabetes, and cardiovascular disease.
It is a familial disease with multiple genes associated with its passing from mother to child. The exact mechanism of this is not understood because of the different manifestations of the disease. However, the environment and other non-genetic factors have a big influence on its manifestation.
Symptoms
- Irregular menses (skipped months followed by excessive bleeding)
- Excessive body hair called hirsutism. Hair may abnormally appear on the face (chin, upper lip), on chest, abdomen and excessively on limbs
- Acne due to excess male hormones
- Thinning of hair and male pattern baldness
- Irregular ovulation leading to difficulties conceiving
- Excess weight and difficulty in losing weight
PCOS is a chronic disease without a cure. Treatment includes lifestyle changes (weight loss, 30 to 60 minutes of daily exercise, low-carbohydrate, low-fat restricted diet), hormonal medication to make menstrual cycle regular and to lower male hormones which in turn reduces hair growth. Creams and laser treatment can also deal with excess hair. The woman is given medication to induce ovulation, combined with insulin sensitising drugs to improve effect. Hormonal injections also induce ovulation. If ovaries are resistant to these treatments, surgery can be done. In vitro fertilisation may be another option.
***
Causes of male infertility
Brain: Hormonal disorders: Improper function of the hypothalamus or pituitary glands in the brain that produce hormones that maintain normal testicular function.
Too much prolactin, a hormone made by the pituitary gland or other conditions that damage or impair the function of the hypothalamus or the pituitary gland may result in low or no sperm production.
Tumours and growths can affect the male reproductive organs directly, through the glands that release hormones related to reproduction, such as the pituitary gland, or due to unknown causes.
Brain: Stress can interfere with certain hormones needed to produce sperm. Severe or prolonged emotional stress, including problems with fertility, can affect sperm count.
Drugs: Anabolic steroids taken to stimulate muscle strength and growth can cause the testicles to shrink and sperm production to decrease. Use of cocaine or marijuana may temporarily reduce the number and quality of sperm.
Exposure to radiation or x-rays can reduce sperm production, though it will often eventually return to normal. With high doses of radiation, sperm production can be permanently reduced.
Advanced age: After age 40 men are more likely to report difficulty conceiving.
Antibodies that attack sperm by mistakenly identifying sperm as harmful invaders and attempt to eliminate them.
Genetic disorders which may cause no sperm to be produced, or low numbers of sperm to be produced e.g. Klinefelter syndrome where a boy is born with two X chromosomes and one Y chromosome (instead of one X and one Y). This causes abnormal development of the male reproductive organs.
Obesity is associated with lower volume of semen, sperm count, concentration, and motility, as well as greater sperm defects.
Side effects of treatments such as testosterone replacement therapy, long-term steroid use, cancer medications (chemotherapy), certain antifungal medications, and some ulcer drugs can impair sperm production.
Exposure to environmental toxins such as pesticides, heavy metals like lead, cadmium, or mercury, as well as aflatoxins in food.
***
Nairobi-based fertility expert Dr Jane Machira provided information for this story.



