World Aids Day: Communities make the difference
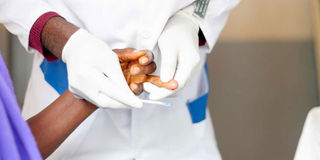
Trained peers or community health workers can deliver rapid diagnostic tests with same day results. PHOTO | FOTOSEARCH.
On 1 December every year, the international community comes together to mark World AIDS Day.
This year’s theme is “communities make the difference”, in recognition of the essential roles that local leaders, networks of people living with HIV, peer educators, community health workers, civil society organisations and grass roots activists play in the AIDS response. Communities ensure that the response remains relevant, grounded and centred on people. Of the estimated 26 million people living with HIV in Africa in 2018, four out of five (81 per cent) get tested, two out of three (64 per cent) get treatment, and one out of two (52 per cent) achieve viral suppression with no risk of infecting others. Across the region, new HIV infections continue to decline, and we are making progress towards elimination of maternal-to-child-transmission of HIV.
COMMUNITIES
Key to this work, are millions of community members, many of whom are living with or affected by HIV. Countries like Rwanda and South Africa have shown how trained peers or community health workers can deliver rapid diagnostic tests with same day results, enabling more people to know their HIV status. Initiatives across the region show that people are more likely to continue with HIV treatment when peer educators counsel and support each other. Community members in Benin, mentor mothers in Lesotho, adherence groups in Mozambique, community pharmacists in Nigeria, and adolescent treatment supporters in Zimbabwe continue to improve linkages to care, adherence to treatment and overall well-being of people living with HIV.
In Zambia, an intensive door-to-door effort in selected peri-urban communities by community health workers, to promote and provide a range of HIV and health services has achieved the 90-90-90 testing and treatment targets and dramatically reduced new HIV infections by 30 per cent in the target communities. [The 90-90-90 is a 2020 target to have, 90 per cent of all people living with HIV will know their HIV status. 90 per cent of all people diagnosed HIV infection receive sustained antiretroviral therapy and 90 per cent of all people receiving antiretroviral therapy have viral suppression.]Despite this success, 1.1 million people are infected with HIV every year in Africa. Together, we must address several challenges to end AIDS by 2030. Funding for the AIDS response is reducing, putting our progress at risk. The coverage of HIV services is still not universal — those in greatest need suffer the most.
AT RISK
Adolescent girls and young women continue to be at higher risk of HIV infection due to gender inequalities, gender-based violence, early marriage, transactional sexual relationships and other harmful cultural practices. Men are less likely to take an HIV test and to initiate HIV treatment. Most children living with HIV are not accessing treatment. Stigma and marginalisation persist, especially among those at highest risk of infection. Overcoming these challenges requires a community-led approach, reaching beyond health facilities. Communities must be empowered to drive change by increasing their access to knowledge, rights and power. As WHO, we recommend a mix of approaches for testing, including community-based testing, self-testing and provider-assisted referral to reach people at highest risk. We also recommend that countries train and mobilise community health workers, including people living with HIV, to provide decentralised and differentiated HIV care and treatment.
Today, I call on governments and donors to continue investing in the AIDS response in Africa. The recent replenishment of the Global Fund was a welcome demonstration of global solidarity. In closing, communities are the heart of the HIV response and I ask that you continue to advocate for universal access to HIV services, to help create demand for HIV services, to influence national HIV policies, and to provide HIV prevention and treatment to those you serve. You are making the difference, to end AIDS in our lifetime.
Dr Matshidiso Moeti is the WHO Regional Director for Africa.


