Cuban doctors not the answer to lack of local specialists
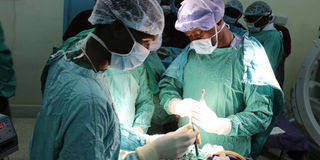
Without making health infrastructure available, you cannot retain specialists in rural areas, whether the specialist is Kenyan or from Cuba. PHOTO | FILE
Every year, at least 500 high school leavers are placed in medical schools around the country, at the behest of the government.
These students pay a subsidised fee to be trained as doctors, while the government pays for the actual cost of training, which is estimated to be at least Sh500,000 per student per year, for six years.
COST OF TRAINING
The government also foots the cost of internship for these trainee doctors.
That we don’t have enough doctors in hospitals, is not in question, even though we have made great strides in training home-grown doctors.
We are now training and graduating almost 1,000 doctors locally and abroad every year and we are steadily working towards the 1:1,000 doctor to population ratio recommended by the World Health Organisation (WHO).
It is worth noting that only about 55 per cent of all WHO member states meet this requirement, with none in sub-Saharan Africa.
For a country with 10,921 registered doctors and at least 7,000 of them in active practice, our doctor to population ratio is no longer the 1:16,000 that the government is clinging on, but rather 1:5,700.
What is baffling is that though the government claims a doctor to population ratio of 1:16,000, it refuses to employ 1,200 fully qualified, but unemployed doctors at its disposal, probably the biggest waste of resources, given the amount of money the state spent on training them.
Now the government has signed a deal with Cuba to bring in 100 specialist doctors to provide medical care in rural areas.
SPECIALISTS
It is good that we recognise the need for specialists, but we must also acknowledge our failure to invest in training local specialists.
Doctors have misgivings about the government’s willingness to employ foreigners for jobs that local doctors are trained to do, yet the government has refused to employ them.
Since 1973, Kenya has had capacity to train most major specialists.
However, unlike countries that invest in healthcare and where every registered doctor is viewed as a potential specialist and encouraged to train further, Kenya trains less than 100 specialists annually and this number has not grown despite the number of newly graduating doctors growing exponentially and the population exploding.
Is it really cheaper to import specialists at a much higher cost than our own locally-trained ones?
RURAL POPULATIONS
Of all arguments fronted by the government, the strongest yet is the need to provide rural populations with access to specialised care. I strongly support this argument, but diverge on the how. First there is need to define “rural”. As it is, every one of our 47 counties boasts at least one county referral hospital at level 4 or level 5.
None of these facilities are in rural areas. All these hospitals are in the major towns of counties, which may not be at the same level, but by all means are in urban settings. These hospitals are staffed by Kenyan specialists, whose numbers fall short.
The populations that are rural enough to lack access to specialists are suffering from lack of health facilities to begin with. Where facilities that can accommodate a specialist in rural areas exist, they are faith-based rather than government-owned.
An example is AIC Kijabe Hospital, a mission hospital deep in the bowels of rural Kijabe in Kiambu County. In spite of its location, Kijabe has a full complement of specialists and super-specialists.
Let’s be honest: without making health infrastructure available, you cannot retain specialists in rural areas, whether the specialist is Kenyan or from Cuba.
No self-respecting cardio-thoracic surgeon will attempt to do a heart transplant in an operating room that does not meet the requirements for such a procedure. Moreover, such a hospital will likely lack a proper intensive care unit for the patient to recuperate in.
CUBAN DOCTORS
We can bring in all the high-level specialists we can afford, but the challenges the Kenyan specialist doctor will face in my home county of Nyamira will be the same ones awaiting his Cuban counterpart.
The Cuban doctor will face additional difficulties in language barrier, ignorance on disease patterns, socio-cultural beliefs that present barriers to healthcare provision, rampant corruption that leaves our facilities without consumable products (like medical gloves, syringes and needles, tubes and catheters) for use in patient care, broken down systems that will fail the doctor in their endeavour to provide the best possible care and lack of support from other non-medical sectors that must work in tandem to ensure successful healthcare provision.
My first medal of honour will be to the Cuban paediatrician who figures out what “macho mbaya” means when a mother in rural Busia brings in their feverish seven-month-old baby, but stubbornly refuses any injectable drugs.
We also await to hear success stories of surgery conducted in Tana River to save a little boy who has been mauled by a crocodile when the county is plunged into a 72-hour power outage and there is no diesel for the generator.
Let’s remember that we are importing doctors, not the twelve disciples to perform miracle healing! As we celebrate Labour Day, let’s think about the role of the government in empowering and protecting its own local workforce.



