How WhatsApp is helping diabetics gain back their health
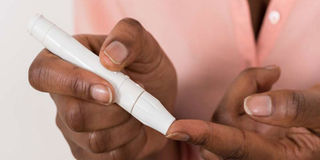
How to check blood sugar level with a glucometer. PHOTO | FILE | NATION MEDIA GROUP
Upon seeing George Juma training for rugby matches, one may not realise that he struggles with diabetes (type 1) every day.
He was diagnosed three years ago after being taken by the invisible force of high blood sugar, while playing the game he loves – rugby.
As part of staying healthy and leading a full life in spite of the condition, he is also an active member (one of the youngest) of a diabetes support group on WhatsApp.
George Juma is typing ...
“I will be out on loan to Shamas Rugby now that I am done with KCSE,” he updates the group members, something that is followed with a series of congratulations and a rainstorm of emojis.
According to the administrator, Duncan Motanya, the founder of the Diabetes Management Resource Centre, the social media support group goes beyond medication as a means of managing the condition, by bringing together patients to share challenges, nutrition and physical activity tips.
“The condition is easier to manage with a support system. Our goal is to help members learn about diabetes, make healthy eating and physical activity part of their daily routine in addition to following doctors’ instructions of keeping blood sugar within target levels,” Motanya says.
RESISTANT TO INSULIN
Here’s how a typical day in the group goes (in this case World Diabetes Day on 14th November). The theme is Women and Diabetes:
Esther Catherine is typing … as the rest wait patiently to see what she will say.
After getting pregnant three times and having miscarriages every time, Esther decided to see a gynaecologist to find out what the problem was. The first doctor told her it could be due to working too hard and on strenuous activities, but that answer did not satisfy her.
The second doctor was more thorough. He painstakingly took down her health history and family history and had her take several tests to ascertain what the problem was. Her father and elder brother were diabetic, and her results showed that she was diabetic too.
Gestational diabetes is first diagnosed during pregnancy. Similar to type 1 and type 2 diabetes, gestational diabetes causes blood sugar levels to rise above normal.
When a woman is expectant, the body becomes resistant to insulin. This is to allow more provision of glucose to nourish the baby in the womb. This is not threatening for some mothers.
When the body signals excess production of glucose the pancreas secretes insulin to breakdown excess glucose.
However, when the rate of glucose production supercedes the rate at which the pancreas releases insulin, there is a rise in glucose levels. This results in gestational diabetes. This is why women should have blood sugar checks during pregnancy.
PUT ON BEDREST
If a woman with risk factors such as obesity, family history of diabetes or gestational diabetes realises she is pregnant, she should have her blood sugar levels checked immediately, because if not caught and treated promptly, gestational diabetes can cause health problems for the mother and baby.
Women with gestational diabetes are at an increased risk of complications during pregnancy and delivery and though gestational diabetes is not permanent, mothers who experience it and their children are at an increased risk of future type 2 diabetes.
Once Esther realised what was causing her miscarriages, she was put under close monitoring, told to watch her diet and get frequent check-ups.
At around week 11 of pregnancy, she was put on bedrest to save her pregnancy after a scare.

An insulin shot. PHOTO | FILE | NATION MEDIA GROUP
One month to her expected delivery date, she was put on insulin. When she went into labour, she developed complications and delivered a 3.8 kg healthy boy via Caesarean section. After a while, her blood sugar normalised and she went off the insulin.
The next year she had another miscarriage, but after that she went on to have eventful, but closely monitored pregnancies and she delivered two other babies.
Her third baby was born at term in October 2008, but weighing 1.15 kg which was odd because most diabetic mums give birth to big babies.
The baby was ready to go home after 30 days in an incubator, and Esther continued to struggle with post-gestational diabetes for the years that followed.
Esther’s long narration is followed by threads of emojis representing various emotions from strength to applause and encouragement, and a torrent of “Amens.” There is no sadness, just cheers.
KENYAN DIET
In the group are also specialists who answer questions posed by members. And when they are not sharing their experiences, the patients encourage each other and remind each other to exercise.
“I learnt almost everything I know now from this group and I have not visited any hospital since I joined nine months ago. I am now very healthy and I monitor my blood sugar regularly,” says 24-year-old Bery Makungu, a member of the WhatsApp support group.
The nutritionists in the group also offer tips and answer questions on what to eat to manage diabetes. The advice extends to family members of the group members who are now nutrition ambassadors in their households.
Sadly, the typical Kenyan diet is high in carbohydrates moderate in protein and very low in vegetables and fruits. “We eat high-energy foods and consume very few micronutrients (vitamins, minerals and phytochemicals).
This coupled with lack of exercise leads to corresponding obesity, belly fat, reduced insulin sensitivity and eventually diabetes,” says Stella, a nutritionist in the group.
SEDENTARY LIFESTYLE
“To prevent diabetes, effectively manage it and prevent onset of complications, we must adopt healthier lifestyles and healthy meal planning. If we don’t make food our medicine, medicine will be our food.”
Wathoya is typing …
Another morning, another day to talk about diabetes. She is a victim of a poor diet that spiralled down to diabetes complications. Now a mother of two, she was diagnosed with diabetes in 1998 at the age of 27.
“My sedentary lifestyle, poor eating habits and the resulting obesity likely contributed to the onset of diabetes. We didn’t have a family history of diabetes then … now we do,” she types.
Even after diagnosis, irregular follow-ups and a care-free diet put her in and out of hospital. Then in 2007, she realised there was something wrong with her eyes; she couldn’t see as clearly as she used to. And then her kidneys collapsed.
“That is when the reality of the living nightmare I was in began,” she recalls. Despite financial constraints, her family hurriedly organised for a kidney transplant in India in January last year.
“I now lead a healthier life with my new kidney which has to be maintained using lifelong immunosuppression drugs that are a tad too expensive and have to be sourced outside the country


