Your final chance to stop a medical apocalypse
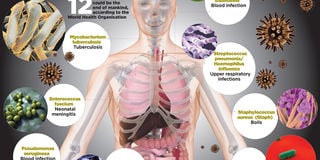
The bacteria listed are divided into three categories based on the urgency with which new antibiotics are needed against them. They’re classified as critical, high and medium priority. PHOTO| FILE| NATION MEDIA GROUP
If you have a virus such as common cold or flu, you feel bad.
The next thing you do is walk into a pharmacy and ask for antibiotics, because you, like your neighbour, believe they can fix everything.
Since the pharmacist is busy, is running a business, and wants you to come back to his shop tomorrow, he hands you the pills and stretches his hand for the Sh100 bill.
You pop the pill and go about your business, wallowing in the fleeting feeling of conquest, that you have solved your problem.
You are wrong. And you, like millions of other Kenyans, are putting the rest of mankind at risk.
Antibiotics are routinely prescribed for infections they do not treat, or for which they are not needed in the first place.
Also called antibacterials, they are used in the treatment and prevention of bacterial infections and are deemed a medical marvel because of the huge way they transformed modern medicine.
However, more often than not, you should not be on them when you are feeling under the weather.
“More than 70 per cent of antibiotics prescribed are either given unnecessarily or used improperly,” says Prof Samuel Kariuki, Director of the Centre for Microbiology Research at the Kenya Medical Research Institute (Kemri).
“You go to a doctor with a cold or flu, and walk away with a prescription for antibiotics!”
And now Man is paying the price of his sins, as this overuse and misuse of otherwise good drugs has encouraged germs (bacteria) to evolve and develop resistance, resulting in the emergence of untreatable “superbugs” that threaten the basis of modern medicine.
ABUSE OF ANTIBIOTICS
Drug-resistant infections are already responsible for an estimated 700,000 deaths every year.
If no action is taken, they are expected to kill 10 million people annually by 2050. Antibiotics are key to preventing both pre- and post-surgery infection.
For instance in Kenya, three in every 10 births are by caesarean section, where antibiotics are used to protect the mother and baby.
Also, since most cancer treatments suppress the patient’s body’s ability to respond to infections, antibiotics, antifungals and antivirals help to keep people alive as they receive routine cancer care.
For these and many other reasons, antibiotics play a crucial curative role in the health sector.
But they are now failing to do what they were designed to do, and scientists, researchers and international health bodies have panicked.
So worrying is the rate of resistance that the World Health Organization (WHO) was in February this year forced to publish a list of the 12 bacteria, which pose the greatest threat to human health because they are resistant to antibiotics.
The first of its kind, the list highlights bacteria that global health experts believe pose the greatest threat to human health.
It was drawn up in a bid to guide and promote research and development (R&D) of new antibiotics as part of WHO’s efforts to address growing global resistance to antimicrobial medicines.
Experts examined a number of criteria, including how deadly the infections the bacteria cause are and whether new antibiotics to treat them are already in the pipeline.
The bacteria listed are divided into three categories based on the urgency with which new antibiotics are needed against them. They’re classified as critical, high and medium priority.
Topping the list as “critical priority” were bacteria that commonly cause hospital-acquired infections, picked up both in hospitals and health care settings like nursing homes, and from patients who require equipment such as ventilators or blood catheters, which can become contaminated.
These bacteria can cause severe and often deadly infections such as bloodstream ailments and pneumonia.
And, according to WHO, these bacteria have already shown resistance to multiple drugs.
“They are responsible for high mortality rates,” says Dr Marie-Paule Kieny, WHO’s assistant director-general for health systems and innovation. “New, effective therapies are imperative.”
DRUGS DEVELOPMENT
Prof Kariuki agrees that there is need to draw up this list.
“The top three (bacteria) do not even have drugs to treat them,” he says, adding: “The main concern is the loss of available antibiotics as doctors are now prescribing last line drugs, which we never thought would be needed this soon. This makes us very worried.”
To treat them, Prof Kariuki says medics will need to use a less-than-ideal drug, known as Colistin, a last resort type of antibiotic... but resistance is also becoming more common.
Other increasingly drug-resistant bacteria, which are deemed high and medium priority, cause more common diseases such as gonorrhea, pneumonia, typhoid and food poisoning.
“These still have some drugs to fight them, but doctors are being forced to use last line drugs because resistance levels are so high,” Prof Kariuki says.
Dr Kieny adds: “Antibiotic resistance is growing and we are fast running out of treatment options. If we leave it to market forces alone, the new antibiotics we most urgently need are not going to be developed in time.”
As a result, the WHO is calling on governments and pharmaceutical companies to prioritise the development of new drugs against them.
***
Mycobacterium Tuberculosis
Tuberculosis
Tuberculosis is an infectious disease that usually affects the lungs, and the bacteria, being airborne, can spread through the air from person to person. Compared with other diseases caused by a single infectious agent, TB is the second biggest killer globally, with an estimated 1.8 million people dying from it in 2015 and another 10 million falling ill. The World Health Organisation estimates that nine million people a year get sick with TB, with three million of these “missed” by health systems. “TB is a poor man’s disease and very common in developing countries. Given that there is already multi-drug and extensively drug-resistant forms, there is need to be very worried as doctors now have to resort to last line drugs,” says Prof Samuel Kariuki, Director of the Centre for Microbiology Research at the Kenya Medical Research Institute (Kemri).
Enterococcus faecium
Neonatal meningitis
This bacteria coexist in the human intestine and have long been recognised as important in humans. They are commonly found where there is fecal matter like sewers or where people practise open defecation, explains Prof Kariuki. But they may also turn pathogenic, causing diseases such as neonatal meningitis — a serious medical condition in infants caused by the bacterial infection of the blood — or a rare and potentially fatal infection of the inner lining of the heart known as endocarditis.
Pseudomonas aeruginosa
Blood infection
This rod-shaped bacteria can cause disease in plants and animals, including humans. Prof Kariuki explains that serious infections caused by this bacteria usually occur in people in the hospital and/or with weakened immune systems. It can be spread on the hands of healthcare workers or by equipment that gets contaminated and is not properly cleaned. “Infections of the blood, pneumonia, and infections following surgery can lead to severe illness and death in these people,” he says. Healthy people can also develop mild illnesses if infected, especially after exposure to water. Patients in hospitals, especially those on breathing machines, those with medical devices such as catheters, and those with wounds from surgery or from burns are potentially at risk of serious, life-threatening infections.
Acinetobacter baumannii
Typhoid, pneumonia
These are a large family of Gram-negative bacteria that include, along with many harmless symbionts, many of the more familiar pathogens such as Salmonella, which causes typhoid and Escherichia coli, found in the environment, foods, and intestines of people and animals. Enterobacteriaceae is found in the intestines of animals and is also commonly found in hospitals. When it gets to a patient’s bloodstream, this bacteria can cause various illnesses like pneumonia, bloodstream infections, wound infections, meningitis or urinary tract infections (UTI).
Acinetobacter baumannii
Blood infection
This is a typically short, almost round, rod-shaped bacterium. It is an opportunistic pathogen in humans, affecting people with compromised immune systems, and it is becoming increasingly important as a hospital-derived infection. While other species of this bacteria are often found in soil samples, it is almost exclusively isolated from hospital environments. In Kenya, this bacteria is common in Intensive Care Units (ICUs) and among patients undergoing long-term treatment. “Depending on the primary cause of hospitalisation, it may be worse,” says Prof Kariuki.
Streptococcus pneumonia/ Haemophilus influenza
Upper respiratory infections
These type of bacteria mainly cause illness in babies and young children. They often cause upper respiratory infections such as pneumonia, ear infections, sinus infections, and meningitis, among other illnesses. Whereas the WHO has listed these two among the list of priority pathogens where research and development of new antibiotics is required, Prof Kariuki says that introduction of vaccines against them has significantly reduced the need for treatment, therefore antibiotics are not used so much.
Staphylococcus aureus (Staph)
Boils
Long recognised as one of the most important bacteria commonly found on humans, it is the leading cause of skin and soft tissue infections such as boils (abscesses), boils of hair follicle (furuncles), and infection of the deeper layers of skin and the underlying tissue (cellulitis). Although most staph infections are not serious, this particular one can cause serious ailments such as bloodstream infections, pneumonia, or bone and joint infections. It can also cause food poisoning. According to Prof Kariuki, this particular bacteria, although listed in the WHO’s priority list, is not of very high importance in Kenya.
Salmonellae
Typhoid
Salmonella causes typhoid, an infectious disease spread by contaminated food and water. About 22 million cases of typhoid fever and 200,000 related deaths occur worldwide each year. Most persons infected with salmonella often develop diarrhoea, fever, and abdominal cramps 12 to 72 hours after infection. The illness usually lasts four to seven days, and most people recover without treatment. However, in some, the diarrhoea may be so severe that the patient needs to be hospitalised. Prof Kariuki categorises it as among bacteria that are of high importance for Kenyan scientists. “We have noticed up to 15 per cent resistance to antibiotics, and it is because it keeps adjusting itself to become resistant,” he says.
***



