Falls, burns and bites: Preventable injuries that have children fighting for their lives
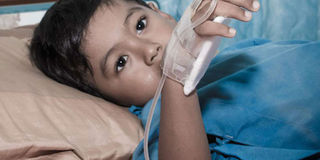
Doctors say the pain and death of the victims is largely preventable, if only there was consideration for child safety. PHOTO | FOTOSEARCH
Dr Joel Lesan stands at the door of Ward 4D at the Kenyatta National Hospital watching children play.
He motions us to stand by the door, then breathes in and sighs.
“Look,” he says, pointing to what has caught his attention in the ward which houses children with burns.
“Without prompt hospitalisation, there is a three in four chance that a child with such a burn will die.”
Some of the children have serious burns, with 25 per cent or more of their bodies burnt.
With a distant look, the paediatric surgeon and head of special surgeries at KNH narrates the story of each child, written on their injuries, scars and fractures.
Baby Martin* was thirsty and innocently reached out for a jug of water on a table.
He poured it into his mouth, sustaining burns in his mouth, throat, chest and abdomen from the hot water in the jug. Apart from the pain, he has difficulty breathing and has to be assisted.
Kevin*, another patient, has his neck joined to his shoulder after a burn, and all the love, patience and tenderness of the nurses dressing his wound do nothing to ease his pain. Constant pain every day. For more than two months.
Dr Lesan would like to operate on the neck, and graft skin from some parts of his body so that he looks normal should he get better, but not now. He needs to heal before his body can endure that.
Then there is Brian* who got burnt when a curtain at home caught fire when his mother stepped out briefly.
PERFORATIONS IN GUT
In this ward are babies who have swallowed batteries. The negative and positive elements react in the tummy, leaving perforations in the gut.
Then there are those who were brought in with breathing problems after inserting a bead in their nose.
There is Dee*, who fell from the third floor and Baby Newton*, who plays happily on the corridor, healed and happy, but unaware that this is not where he should be. His parents left him here, exposed to the risk of catching a hospital bug and falling ill again.
There are wincing children with bandages wrapped all over their bodies.
The children in different stages of healing, peer curiously at passers-by. Many have been referred from other county hospitals such as Mbagathi and Mama Lucy, which do not have wards for burns and bone injuries, or the expertise to handle the cases.
There are also some from neighbouring counties.
This is not a public hospital problem alone.
At Aga Khan University Hospital in Nairobi, children with unintentional injuries are increasingly being wheeled in, with seven out of 10 cases (65 per cent) being boys.
SUSTAINED AT HOME
Most of the injuries (42 per cent) are sustained at home, with apartments and estates accounting for 26 per cent of the cases.
Nearly half of the children sustained serious injuries from falls (56 per cent), and many end up with amputated limbs, deep lacerations and organ injuries.
At Kisumu’s Jaramogi Oginga Odinga Teaching and Referral Hospital, chief executive officer Dr Peter Okoth, says that the most common cause of injuries in children brought to the hospital are snake and human bites.
“Last year we had 233 snake bite and seven human bite cases. The snake bites are mostly in the rural areas. And when children are playing and fighting, it is common for them to bite one another,” Dr Okoth told HealthyNation.
In 2018, the hospital saw more than 1,000 children, of whom 237 were brought in with burns, while 156 had injuries from accidents.
Head injuries were common, as was poisoning often from ingesting cleaning solutions such as bleach or medications prescribed for other purposes.
Health workers fear that the children who are brought to hospital are just a fraction of the victims.
Back at KNH, Dr Lesan says that the children who are brought in to hospital with injuries from accidents are victims of living standards – social and development issues that society can fix to keep them out of hospital wards.
Each child is here because of a larger developmental issue that they had no part in creating. Poverty and high unemployment rates sees families squeezed into little one-roomed spaces in which everything takes place – cooking over an open flame, sleeping, intimacy and everything else.
According to the Kenya Demographic Health Survey (2014), more than half (53 per cent) of households use one room for sleeping and more than half (56 per cent) of them use wood as their main source of cooking fuel. Paraffin is also used, and it is often contaminated with diesel and petrol – a potentially explosive mix.
In low-income estates where many such families are housed, the face is changing from horizontal to vertical, as flats as high as six floors replace other houses in the constraints of space.
As construction workers break wood and stones on the unfinished second and third floors of a flat under construction, children play on the ground floor, where they live, oblivious of the risks.
During the day, babies crawl on the ground, where they risk being hit by falling stones and other heavy objects.
In the evening, the older ones climb up to play football or run in the floors under construction.
Many end up with broken bones.
We find them in another ward, where Dr Sam Njiru, a paediatric neurosurgeon, treats them.
“The ball goes over the wall, and a child running after it, falls to his death or suffers very serious injuries,” says Dr Njiru.
With corruption and laxity in inspecting construction sites for safety, the chain of horror continues: patients stream into hospitals, parents lose their sons and daughters, and children are maimed for life.
Even when the construction is complete, Dr Njiru says, the houses are still not “baby safe”.
The grill on the balcony ought to be small enough that a baby’s head cannot go through, and tall enough that they cannot climb over. But to save on space and money, developers disregard these basic safety rules.
Thirteen contractors in Nairobi, Kisumu, Eldoret and Nakuru contacted by HealthyNation, said that they did not really consider the safety of children during construction.
When asked about their considerations during construction, three contractors from Nakuru said that the wellbeing of children, as opposed to money and space, crossed their mind.
One in Nairobi said that if a parent felt unsafe in his houses, she should leave it for tenants without children. “I do not build houses to act as a playground for children,” he said.
The landlords might not care much, but that little omission of not adding an extra bar to the balcony barrier, costs lives, and you, the tax payer, billions in shillings to treat the victims.
“Every time I look at these children on the operating table, knowing very well that their injuries could have been avoided, I feel very angry.
“They are victims of carelessness and greed,” says Dr Hamdun Said, a surgeon at KNH who handles the children after they are stabilised at the Accidents and Emergencies unit.
“It is very painful not to know what that baby would have become in future, had that accident not killed or maimed him or her,” adds Dr Njiru, with a tinge of regret.
He remembers Baby George*, whose face was cut off in a motorbike accident.
His mother had no health insurance and could not afford to pay for treatment. At the Accident and Emergencies unit, four doctors were called to work on the baby on the table.
The neurotrauma surgeon opened up his skull to drain the confined blood and ease pressure on the brain, and to remove clots; the plastic surgeon patched the chopped face up; the orthopaedic surgeon fixed the bones; the intensive care unit (ICU) nurse waited to take the child to ICU where he would need round-the-clock care to assist him to breathe.
In the ICU, drugs were administered intravenously to prevent convulsions.
The hospital fed and housed the mother during the hospital stay.
In just two weeks, the hospital bill would amount to millions, and because the mother had no health insurance and couldn’t afford to pay, the hospital would have to write the bill off.
This financial cost to the health system deprives it of the resources to offer other services.
“You cannot ask the mother for the money, and the government will not pay the bill … we have to survive. That is not good to hear if we are to talk about it,” says Dr Njiru.
As the status quo continues, Juhudi, the children’s ward, remains crowded and the nurses and surgeons are burnt out, given that there are few specialised trauma experts.
***
Dr Njiru: How society can make environments baby-safe
Cover manholes
Careful who you live your child with. When I conduct X-rays I see children with unexplained wounds, fractures at different stages of healing
Store bleaches, acids and other dangerous liquids and beads away from children’s reach
Have grills on your balconies
Keep children away from the kitchen
No sharp edged furniture
Have door stoppers; doors sandwich children’s arms, causing cuts
Each local hospital should have trauma experts to preserve life of the child by securing airways, and stopping blood loss
Police vehicles should be fitted with emergency medicine kits; they can go through traffic quicker and hence transport children faster
Verah Okeyo



