Poor referral mechanisms to blame for late diagnosis
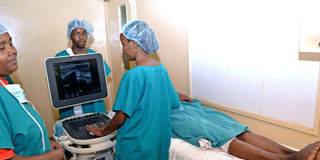
Aga Khan University Hospital's Dr Rose Ndumia (r), does an ultrasound guided breast biopsy on a patient at Nyeri Provincial General Hospital during a free clinical screening for breast cancer in 2012. PHOTO| FILE| NATION MEDIA GROUP
Poor referral measures, lack of diagnostic facilities and inadequate knowledge on cancer by most healthcare providers is a major contributory factor to misdiagnosis and late treatment of cancer.
Take for the case of 45-year-old Eunice Javoga; she was first misdiagnosed with the ovarian cyst instead of cervical cancer the back in January 2015. It took her a second screening which was conducted after three months in April that same year.
“The gynaecologist had initially told me that I had cyst. Previously I developed unusual excess bleeding during my menses,” she added. And although she was later reached stage 2, she believes that the condition treated early.
Prof Chite Asirwa, an oncologist at Moi Teaching and Referral Hospital (MTRH) said that although patients present themselves, healthcare facilities still require more diagnostic facilities to conduct proper screening.
“Quite often we keep reporting that patients present themselves very late to health facilities, but that is not true from our data.
“We have discovered that patient can visit healthcare facilities up to 16 times seeking answers, before they are referred to a hospital that is able to handle their case.
“Most of the time, these patients are diagnosed with tuberculosis instead of lung cancer . . . our feeling if we do mass awareness and screening and embed this in the healthcare system we will end up with more survivors and community have more trust in our health care,” said Prof Asirwa, also Ampath’s Oncology and Haematology programme director during recent summit in Eldoret town to discuss how to tackle emerging issues in the health sector.
NEED FOR TRAINING
The experts also rooted for more training of the health workers like lab technicians, radiologists and pharmacists to understand how to screen and diagnose the patients to weed out misdiagnosis.
They also pushed for more polices to weed out quacks who promise to treat cancer within months or days.
“Most centres have ultra-sound machine but lack good pathology service to do good biopsy. Most hospitals take to private hospitals but if we want to make it affordable to most citizens we need ramp up capacity in terms of lab facilities and health workers. We need to move like other countries and personalised care so that the drugs are readily available to the patient,” added Prof Asirwa.
Cancer and blood specialists maintain that frequent check-ups for cancer is the best approach for early diagnosis and management.
Oncologists highlighted and identified cancer symptoms which one should look out such as fatigue, weight loss, skin changes, lumps, unusual bleeding, pain and high fever.
According to statistics from the Ministry of Health, cancer is the number three killer of Kenyans in the country.
National Cancer Institute’s director, Dr Alfred Karagu said they are engaging the National Health Insurance Fund (NHIF) to ensure that the fund’s packages cover from screening to rehabilitative treatment.
“There are areas that require improvement because we feel there are areas that have not been well covered. We want to ensure members screening, diagnostic, treatment, and even rehabilitative treatment for women who lose breasts are supported to get prosthesis,” noted Dr Karagu.



