Self-testing is a milestone in the war on HIV
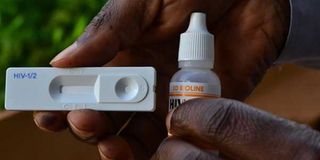
A laboratory technician displays a Bioline HIV testing kit. Kenyans can now take a HIV test in the privacy of their homes using an oral testing kit or a blood test kit. PHOTO | JOSEPH KANYI
What you need to know:
- More importantly, it is expected that self-testing will provide access to knowledge of HIV status to populations such as men who seldom visit health facilities and will enable key populations such as sex workers to offer testing to their clients.
- There is no doubt that scaling up this intervention will be fraught with challenges. At the moment, the available testing kits are overpriced but it is anticipated that the market will respond to increased demand by lowering the cost of the HIV self-testing kit to the price of pregnancy kits or emergency contraception. This will enable a private sector market to thrive further increasing access.
After a decade of scientific debates, community engagement and regulatory approvals, Kenya finally adopted HIV self-testing for people who want to know their HIV status in the privacy of their homes, offices or even at community clinics.
When this kind of test was first proposed in 2007, the major concern was whether an ordinary Kenyan would have the competence to conduct a HIV test and interpret it, and whether they would seek medical attention if they turned out to be HIV-positive. These doubts have now been put to rest with convincing evidence that is not only relatively simple, but is also acceptable among healthcare providers and patients. The issue of potential abuse by individuals who might force their sex partners to take the test without their consent was also raised.
In addition, there was the fear that self-testing might encourage unsafe sex leading to an increase in unplanned pregnancies, sexually transmitted infections and social delinquency.
These issues still linger and we have to establish mechanisms to ensure that this new approach does more good than harm.
Nevertheless, self-testing comes with exciting opportunities. First of all, the practice of public health cherishes individual autonomy. With self-testing, individuals have the opportunity to make choices about how and when to take a HIV test as well as the frequency of testing.
FRAUGHT WITH CHALLENGES
Individuals and families now have the ability to plan for their health and make decisions in a timely manner.
Self-testing will remove the burden of providing this service from healthcare workers who are already constrained by many tasks at health facilities. Also, it will no longer be necessary to queue at a Voluntary Counselling and Testing (VCT) centre, thus saving time for Kenyans who have other social and economic responsibilities.
More importantly, it is expected that self-testing will provide access to knowledge of HIV status to populations such as men who seldom visit health facilities and will enable key populations such as sex workers to offer testing to their clients.
There is no doubt that scaling up this intervention will be fraught with challenges. At the moment, the available testing kits are overpriced but it is anticipated that the market will respond to increased demand by lowering the cost of the HIV self-testing kit to the price of pregnancy kits or emergency contraception. This will enable a private sector market to thrive further increasing access.
Still, the health system has to be tweaked to enable those individuals testing positive to receive a confirmatory test at the earliest opportunity and access HIV counselling and treatment in a timely manner. It may require innovative mechanisms like the use of biometrics, phone applications, call centres and a centralised database to enable the Ministry of Health and county health departments surmount this challenge.
Nevertheless, the launch of this important intervention is a milestone in HIV prevention. It will fast-track universal knowledge of HIV status, and contribute to the decline of new HIV infections.
HIV self-testing will support other innovative solutions such as pre-exposure prophylaxis for HIV and lay a foundation for the implementation of other individually-controlled interventions such as microbicides.
Dr Cherutich is the head of the division of strategic health and research at the Ministry of Health and the chairman of the Public Health Society of Kenya


