In 'country of strikes', Health Service Commission is crucial
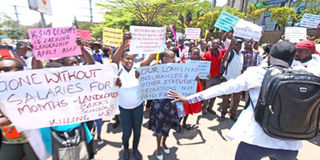
Health workers demonstrate in the streets Kisumu town on September 18 in protest of delayed salaries. PHOTO | FILE | NATION MEDIA GROUP
Across the country, hospitals are grappling with a severe shortage of health workers across all cadres and county governments are unable to hire more staff due to budget ceilings.
The inability to meet the human resource for health has created a gap in service delivery that in turn impedes the delivery of primary healthcare.
Health workers pay has also played a big role in the sector with many counties like Kisumu, Mandera, Kirinyaga, Laikipia, Mombasa and Taita-Taveta failing to implement a 2017 collective bargaining agreement (CBA).
Kisumu County, for example, one of the counties being looked at for lessons for the national roll-out of UHC, was in total paralysis for 90 days (August to October) after doctors and nurses went on strike, citing a harsh working environment and demanding a salary increment.
Since the devolution of health services in 2013, the public health sector has been affected by frequent short and often localised strikes. In 2017, for example, the country experienced a total of 250 strike days in a span of 11 months after a public-sector nationwide doctors’ strike lasting 100 days and then the nurses downed their tools for 150 days.
This year, nurses in more than 20 counties went on strike in February as well as clinical officers for reasons ranging from failure to implement their CBA to salary delays.
CONFLICTING FUNCTIONS
Kenya Medical Practitioners, Pharmacists and Dentists Union (KMPDU) deputy secretary-general Chibanzi Mwachonda says the turmoil is attributed to the mismanagement of workers across the counties, lack of medical supplies and inadequate financing of the sector.
“There are salary delays despite timely disbursement of monies to counties, non-remittance of statutory deductions including PAYE, NHIF and NSSF, deductions to financial institutions including loans and insurance premiums with resultant penalties on the health workers and non-implementation of return-to-work agreements.
While there are no “magic bullets” to avert all problems in the health sector, workers agree that a Health Service Commission (HSC) is what the country needs to afford Kenyans quality health services.
The union’s Nairobi branch secretary-general, Dr Thuranira Kaugiria, says the commission, which could among others advise the national and county governments on policy formulation, human resource planning and deployment, is what the country needs to address the issues in the sector.
“The commission will use the World Health Organisation Workload Indicators of Staffing Need method which provides health managers a systematic way to make staffing decisions in order to manage their valuable human resources well,” he says.
He adds that the commission would not have conflicting functions with devolution since it would only touch on matters relating to the health workers and no other health functions.
“All issues that surround healthcare workers would be sorted out by a central body and unions would engage one central employer instead of 47 counties. This way, we will not see strikes popping up because there is a standardised way of doing things,” says Dr Kaugiria.
FINAL DRAFT
Kenya National Union of Nurses Secretary-General Seth Panyako says the Constitution had the provision for a Health Service Commission, but the failure to include it in the final draft was a huge disappointment. “If we have the HSC, 80 per cent of the problems in the health sector will be solved. This independent commission is something we fully support,” he says.
The commission will be modelled on the Teachers Service Commission. Various countries have established health commissions. Uganda, for example, established one in 1998 to address unique human resources issues.
The commission is mandated to confirm, promote and review the terms and conditions of service, training and qualifications of health workers.
Uganda’s HSC jurisdiction covers central government health institutions which include Ministry of Health and specialised institutions under it such as the Uganda Blood Transfusion Services, Uganda Cancer Institute and Medical Professional Councils which have made the health services in the country seamless.
Nigeria, which has one of the largest stocks of human resources for health in Africa was grappling with a similar crisis and established a commission to effectively deliver essential services.
The commission ensures manpower planning development and training of hospital employees. It also recruits and promotes public hospital employees as well as maintains a comprehensive database of all grades of employees.
It also compiles for gazette publication of establishment matters, staff movement including new appointments, promotions, retirements and dismissals.



