CHESOLI & MAJE: Why post-Covid-19 mitigation must have disaster prevention at its core
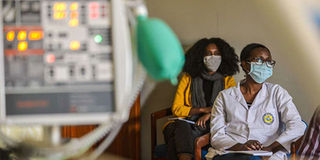
Ethiopian doctors being trained on use of mechanical ventilators for Covid-19 patients. PHOTO | MICHAEL TEWELDE | AFP
What you need to know:
- Social distancing, hand hygiene and face masks will not protect us against an infectious disease transmitted by, say, mosquitoes.
- Social distancing, hand hygiene and face masks will not protect us against an infectious disease transmitted by, say, mosquitoes.
The fallout from Covid-19 pandemic could rise to the levels of the World Wars, the Great Depression and the Spanish influenza of last century. Governments are scrambling to mitigate and control its spread even as the response against other threats — such as climate change, terrorism, cyber-insecurity and economic sabotage — has to be preserved and upgraded.
INFECTION CONTROL
Though laudable, some of the current infection control or prevention and treatment measures will not work for an epidemic caused and transmitted by a different infectious agent.
Social distancing, hand hygiene and face masks will not protect us against an infectious disease transmitted by, say, mosquitoes.
Ventilators would not be useful if the next epidemic, which, instead of causing respiratory failure, affects the kidneys — in which case we will need dialysis machines.
So as not to be blindsided by an infectious disease again, we would need adequate stockpiles of antimicrobial agents and vaccines directed against threats.
These include the potential use of infectious disease agents, such as anthrax and plague, by hostile nations and terrorists.
The challenge, however, is to have rapidly scalable domestic production and supply chain capabilities to meet emergency needs — sometimes for items whose need cannot be anticipated or predicted ahead of the actual epidemic.
PERIODIC UPGRADES
Here, public-private partnerships could be a game-changer. Existing stockpiles would need constant replenishment since drugs expire and machines need periodic upgrades.
Interventions such as social distancing, lockdown and curfews come at a cost, which we must check if they are commensurate with the threats.
After all, engineers grapple with how much resilience to incorporate into the design of a structure by weighing the cost against the risk and consequences of any threat.
Since prevention is always better than cure, communities must decide how much to invest in disaster prevention.
The current Covid-19 toolbox may be ineffective against future pandemics but a range of general measures could avert or mitigate their impact.
An adequately funded fit-for-purpose public health infrastructure with a sound grassroot footprint will be critical.
It would be designed to collaborate with the relevant regional and international health organisations and ensure public health measures that come out of centuries of knowledge and experience pertaining to food and water safety and sanitary living conditions are enforced.
FEAR
A constant source of angst in infectious disease practice is the fear of missing the first case, which then goes on to become an outbreak.
Vigilant public health institutions would be on the forefront performing disease surveillance, identifying incipient outbreaks and rapidly instituting control measures.
Detecting disease patterns in real time, bearing in mind that some infectious agents may be novel, could prevent sporadic cases from becoming outbreaks.
Ordinarily, knowledge of a disease, such as transmission patterns and cell and tissue-level damage inform the choice of control measures, treatment and vaccine. However, the explosive nature of Covid-19 has necessitated reliance on “make-shift” science instead of well-performed research.
There is no assurance that future work may not prove the current control and mitigation efforts to be ineffective or even counterproductiv — thus the need to rapidly scale up research and development capacities, harnessing the power of artificial intelligence.
COVID-19
Covid-19 has affected the private sector and corporations have played a vital role in its prevention and mitigation.
In the post-pandemic world, they should invest in infection control infrastructure and processes, analogous to their investments in physical, cybersecurity and other risks, including in a strong layer of infection control personnel to advise on production and customer care processes.
It is imperative to institutionalise these as well as optimise our overall healthcare infrastructure. Reduction of poverty and income disparities will, obviously, be critical to achieving these goals.
Dr Maje is an infectious disease-trained physician, [email protected]; Mr Chesoli is a developmental economist, [email protected].






