Blood for sale: Why you might soon start buying
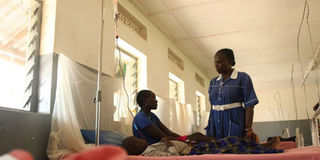
A nurse attends to Chepsera Lemanuk and her son in a hospital in Amudat, Uganda. Chepsera was forced to travel with her son from Kenya to Amudat in search of blood for her anaemic son. PHOTO | VERAH OKEYO | NATION MEDIA GROUP
The heat is licking patients like a hot-blooded serpent in Kacheliba, West Pokot County. Chepsera Lemanuk is hardly noticing it. Her attention is on her severely anaemic son. The boy has been diagnosed with malaria and Kalaazar, diseases that leave him in dire need of blood. But, Kacheliba hospital does not have blood.
Her 200km journey from Sigor in Baringo County to West Pokot in search of treatment for her son is not fruitful. The hospital superintendent Solomon Turkei asks a research van to give her a ride to Amudat in Uganda, 80km away, to get blood.
Chepsera’s son is lucky this time round, but, next time he might not be especially if she does not have money to pay for blood.
While blood donors will still not get paid, as is the common practice in most countries, the blood might no longer be free even in public hospitals from next month.
Blood is crucial in healthcare. Apart from the usual transfusions due to anaemia, there are other conditions that need blood to save life such as bleeding in maternity, cancer patients who need a transfusion after protracted sessions of chemotherapy and accident victims.
SCREEN FOR DISEASES
In Kenya, children under five years and women with pregnancy-related haemorrhage are the most in need of transfusions.
The Health ministry, in charge of blood donation through the Kenya National Blood Transfusion Services (KNBTS), has for the past 15 years relied on the US President’s Emergency Plan for Aids Relief (Pepfar).
Pepfar, which has been supporting blood collection, testing and policy issues in the country, will from the end of this month cut funding, leaving the ministry in a dilemma on how to ensure blood supply is at an optimum.
Health Cabinet Secretary Sicily Kariuki told HealthyNation the “ministry will shift things around to make allocation for the blood services through a supplementary budget. The selling of blood would be a considered option, given that private hospitals already do so despite getting it for free".
She explained further: “We have to figure out if we will sell blood or not sell. Once we decide on that, then we have to figure how to cost it.” The sale, she said, will not be for profit making but for cost recovery.
The cost to the blood transfusion services includes collection of blood which requires storage in sterile blood bags, testing and screening for various diseases as well as storage and delivery of the blood.
By supporting Kenya Pepfar, the cornerstone of US global health assistance, wanted to ensure quality assurance in HIV programmes. KNBTS records show these services were once done at hospitals, and it was cumbersome to ensure the transfused blood was “clean” of diseases.
FUNDING EXTENSION
From 2004 to present, Pepfar has disbursed Sh7.3 billion, which catered for 100 per cent of the services from a centralised point: buildings, vehicles, payment of staff, blood collection and screening for HIV, syphilis and hepatitis C, information systems and even policy guidelines.
Pepfar will not just cease funding on a whim. In fact, HealthyNation has reliably learnt Pepfar turned down Ms Kariuki’s request for a six-month funding extension.
In a phone interview with HealthyNation, the ministry’s communication office said: “Over the last five years, Pepfar has gradually reduced funding to blood safety.”
They further said the ministry is “organising internally and mobilising some funds” to support the service, but did not did not divulge in detail how soon the money will be available and how much.
The US government’s email to HealthyNation about the issue read: “Kenyan government’s commitment to UHC (Universal Health Coverage) is an indication the population will access timely quality services which include blood transfusion. The timing of the Pepfar transition is thus at an opportune time when the Kenyan government’s commitment to sustainable blood service is at its highest.”
The ministry has, however, assured Kenyans will continue to receive the blood as usual.
CHRONIC SHORTAGE
Dr Sophie Uyoga, who has been conducting research at the Kenya Medical Research Institute Wellcome Trust Programme in Kilifi, told HealthyNation Pepfar’s arrival led to the centralisation of the services to ensure quality.
The funding hitch comes at a time the country is already facing a chronic shortage of blood. Blood collection has been plagued by lack of funds for screening tools. There is hardly any money to pay workers to collect and store blood.
An employee at the Kisumu blood transfusion centre, who spoke to HealthyNation on anonymity, said they had run out of reagents and blood bags, which are key in running the blood banks in the region.
“If an emergency happens right now in the county we would be in trouble because the basics of blood donation services are unavailable,” he said.
Aida Odhiambo witnessed first-hand the blood crisis. She was rushed to Jalaram hospital for an emergency caesarean section. Her cousin, Jairo Mchanga, who had accompanied her to offer blood, delivered a note to the facility from the Kisumu blood transfusion centre, asking the hospital to proceed with the procedure.
The Kisumu blood transfusion centre did not take his blood and, instead, asked him to go back at a later date to donate because they did not have blood bags. “They said they do not have the bags and assured me that Jalaram would proceed with the operation with just this note,” he said.
FUEL CARS
Blood services in Kisumu, like other collection centres in the country, are nearly crippled and over time the centre has been forced to look to people of goodwill to keep the blood bank running.
The situation may have come as a surprise for Mr Mchanga, but it has become the norm for employees at the centre that has satellites in Kisii, Migori and Busia as well collection centres in Homa Bay, Vihiga and Siaya.
“One of our drivers is on leave as he awaits confirmation of his employment. We have a good working relationship with the county and we often talk to them to help with fuelling our cars as well as offer donors,” said an employee of Kisumu centre.
Neighbouring Kakamega County is also in the same conundrum. The county government took over blood donation services, but a year into their operation they have hit a snag after they ran out of funds to sustain it.
“The county now looks to the Kisumu centre, which cannot help since its screening process is different. We are worried that should anything go wrong, they (Kakamega) would blame the blood they get from us,” said the employee.
RECORD ERRORS
In Kwale County, the blood transfusion services have not been at an optimum given the location of the facility. There only two schools in the area and the facility put up by Base Titanium is barely surviving given the lack of donors and funds to keep it running.
Bloodlink Foundation Executive Director Joseph Wang’endo said with the total phase out of funding screening will be hard.
“A total of 18 National Testing Laboratories in the country have run out of the automated screening reagent — Abbott 800 — and are now running a manual platform which has slowed down blood screening in hospitals,” he said.
Only two of the six national centres — Nairobi and Nakuru — are currently screening blood, and with the manual process, they can only process 270 units per day as compared to the 800 units when the process is automated. The errors are also high.
“We are looking at a national disaster as safety measures are compromised. Hospitals are using rapid kits and given the costs of screening, some facilities will make it expensive to get blood,” said Wang’endo.
Hospitals such as Kenyatta National Hospital, with a daily transfusion of more than 70 units, get as little as five units a day from KNBTS.
Dr Uyoga said Kenya relies on students, such that when schools close, the shortage is almost felt immediately. Ignorance has been blamed for a low number of adult donors.
“After the outreach, a willing donor fills a form through which they will rule out unhealthy people. Anyone on antibiotics, recently vaccinated, diabetic, suffering from a cold or women with haemoglobin less than 12 or weighs less than 55kg will not qualify. After the collection, the blood is screened.”
MOTIVATE DONORS
Dr Uyoga explained these are HIV, syphilis and hepatitis C are screened due to prevalence.
She said cultural beliefs were also an obstacle to blood donation as some people “fear their blood may be used for witchcraft” or their HIV status would be exposed.
For this reason, the ministry has launched a blood drive this week, and has invited Arjun Mainali — the world’s top donor — to encourage donation.
She said donating blood was beneficial to a donor because there were checks conducted for free and one got to know their blood group.
Dr Uyoga said Kenya had a long way to go.
Citing the example of Nigeria which has a mobile application that reminds donors of the next round of donations, she said embracing technology would encourage the public to give blood.
She said one of the ways to encourage donors would be to put in place a system that could enable them to track their blood from the time of donation to when it helped a patient.
Dr Joseph Mburu, the medical superintendent of Nakuru Level Five Hospital, said he received many emergencies from accidents due to their proximity to the Nairobi-Nakuru highway and closeness to black spots such as Sachang’wan.
He said doctors were forced to “decide at the moment of crisis who would benefit the most from a blood transfusion”.




