Covid-19: What Ebola has taught us
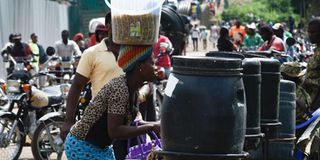
People from Democratic Republic of Congo wash their hands at the Ebola screening point bordering DRC in Mpondwe, western Uganda. PHOTO | AFP
One key take-away that containment of the world's second-deadliest Ebola outbreak has taught us is that viruses do not take breaks.
This was the overriding message health experts and scientists shared as they announced the end of the epidemic, which killed more than 2,000 people and involved the first widespread use of a vaccine against the virus.
The outbreak began in August 2018 and killed at least 2,280 people, around two-thirds of those infected.
It occurred primarily in eastern Congo’s North Kivu province, and to a lesser extent in neighbouring Ituri, where armed conflict, mistrust in aid organisations, widespread corruption, and competing outbreaks of measles and the novel coronavirus have all complicated the Ebola response.
Given the complex situation, Matshidiso Moeti, the World Health Organization’s Africa director, said sometimes ending the haemorrhagic fever seemed like mission impossible. “It wasn’t easy,” said Dr Moeti. “At times, it felt like mission impossible.”
Ebola is endemic in animal populations that reside in Africa’s tropical forests and is passed from person to person through contact with bodily fluids.
Congo has had 11 outbreaks since the virus was first identified in humans in 1976. A new outbreak began on June 1 in the country’s northwest and had resulted in 15 deaths as of June 25. The worst outbreak of the virus swept through Guinea, Sierra Leone and Liberia between 2014 and 2016, killing more than 11,000 people.
Speaking during a virtual conference to announce the end of the outbreak, which the emergency committee declared no longer constitutes public health emergency of international concern, experts reiterated that from the Ebola outbreak African countries can learn a lot on how to handle the ongoing global coronavirus pandemic.
President Uhuru Kenyatta last week lifted lockdowns amid a warning that taming Covid-19 now depends on own individual behaviour, not monitoring by the State. His message was clear: The virus has not been contained, but the economic activities must continue. And it is the individual behaviour of Kenyans that will prevent the further spread of the disease and influence his future actions — including the possibility of rescinding his decision if the Covid-19 cases increase rapidly.
“Let us not lie to each other that the disease is not real. Those who want to use this opportunity to travel home, it is okay. But, remember you are visiting the elderly, who are most vulnerable to the disease. The government will not take responsibility if you infect them. If there is a problem you know that you will be responsible,” he warned during his speech at the steps of Harambee House.
“In the next 21 days we shall study patterns of interactions and the spread of the disease. Any trends that signal a worsening of the pandemic, we will have no choice but to return to the lock-down,” warned President Kenyatta.
FACE STIGMA
So, what lessons can we draw from the Ebola crisis to contain Covid-19?
For starters, good responses outlast outbreaks, says WHO director-general Tedros Ghebreyesus.
Ebola unleashes fear and grief, widely affecting mental health. Survivors also often face stigma and need help to reintegrate into their communities; similar challenges with Covid-19 seem likely, with instances of discrimination seen around the world.
For DRC, having fought the Ebola outbreak better equipped it to address the other health emergencies it still faces, including the current pandemic. The Ebola outbreak led to improvement in public health architecture. Five new labs, part of a recently strengthened surveillance system, will continue to operate. Healthcare workers trained in clinical management and infection prevention and control as part of the Ebola response are being redeployed to fight Covid-19.
A good example is the genome sequencing tool which has seen DR Congo publish the highest number of sequences so far. “When we talk about gene sequencing, then DRC is the country that has given Africa the highest number of sequences because we were able to acquire machines during Ebola. These are the same machines that have been deployed for Covid-19,” said Prof Jean-Jacques Muyembe, the director-general of the DR Congo National Institute of Biomedical Research.
Prof Muyembe, who is also leading the country’s Covid-19 response, however, believes that the spread of the highly contagious, respiratory infections will be best contained by finding an effective vaccine that can be used to obtain herd immunity.
As Covid-19 poses a threat to every region of the world, the DRC holds lessons for countries of all incomes. For example, contact tracers used technology to overcome insecurity, swapping folders of forms for mobile phones to collect data on Ebola, to both help share information faster and ward off unwanted attention in areas where suspicions run high. “The Covid-19 pandemic shows that borders cannot protect us and we are only as strong as our weakest link,” said Dr Ghebreyesus.
In the midst of the outbreak, innovation and research played key roles in ensuring that a vaccine, the first of its kind to be developed and used in a span of five years, was deployed within the shortest time possible. “We have learnt that we can simultaneously deploy important tools as we learn about them,” said Dr Moeti.
ISOLATE PATIENTS
Yet, important as research has been to the Ebola response, engaging communities and influential figures, such as faith leaders and traditional healers, was critical. Communities should be respected as first responders, who can quickly detect cases and collectively work out how to isolate patients, even with minimal resources.
"Countries with governments that communicate complex science directly to the public and use science as a basis for control, have had much better success fighting Covid-19," said Dr Mike Ryan, the executive director of WHO's health emergencies programme at a recent meeting on Covid-19.
For Dr Esto Bahizire, an infectious disease epidemiology researcher, who was involved in the Ebola infection, prevention and control training in one of the regions bordering North Kivu province, some of the loopholes he is seeing in the war against Covid-19 gives him a sense of déjà vu.
“To counter the laxity of the 2014-2016 outbreak in West Africa, international and national health organisations came in with the Land Cruisers and pitched camp in North Kivu. But, to the locals who had been countering rebel groups and a lot of violence, the question was, where were they when we were being raped and killed,” recounted Dr Bahizire.
As the crisis began to escalate, there was a clear sense that people were reluctant to own some of the interventions being introduced to contain the spread of the disease.
“At some point, some of the thinking was that everybody came in to stop this ‘imaginary disease’ because they (the foreigners) were afraid it would spread to their countries,” said Dr Bahizire, currently pursuing further studies and research at the University of Nairobi.
By coming with their own teams of health workers, they sidelined those who had been working with the communities. The organisations eventually had to change their strategies.
Given that the Ebola death rate was much higher than Covid-19, he said, prevention was vital. That meant implementation of strong hygiene and sanitation measures was needed.
But, how do you implement best hygiene practices and specifically handwashing and isolation in a community which perceives you as the outsider and the disease foreign?
WORK WITH COMMUNITY
According to Dr Bahizire, the management of each outbreak is complex and has, among others, a medical and social aspect. “You cannot implement one without the other,” he said.
For this to happen, he opined, we need community engagement. Community leaders must be involved, local health care workers have to take part in the process, the messages have to be tailored in a manner that the community understands. This communication must be sustained for a long period.
Liaising with local authorities and partners would be key. Besides developing health centre infrastructure, how health messaging is tailored and disseminated and the level to which the community is involved will determine whether a disease outbreak is contained or not.
“In North Kivu, something like shaking of hands ended because a church leader advised the locals on the negative effects of contamination. Similarly, mechanics in Dagoretti will be more receptive to one of their own and embrace change than when listening only to someone on the radio or TV talking about Covid-19,” explains Dr Bahizire.
Although the treatment for Ebola is different from what is needed for Covid-19, one aspect is the same: Hygiene. In both cases, Dr Bahizire reiterated, community messaging was desperately needed. And in both cases, if you have symptoms, you must isolate.
While he agreed that Covid-19 public health and social measures amenities like use of masks, sanitisers, and water and soap for hand hygiene must be made available, he noted that in Kenya, they were not being fully observed. In many cases, the measures that have been introduced by the government are perceived to be punitive. Unfortunately, the same thing was happening in some provinces in DRC, he said.
“For example, I have been in matatus where one person is talking on the phone, another is chewing on to their roasted maize, all the while forgetting that they are in a small space with a tight circulation of air. If one of these people has the virus, they can easily spread it,” he said. “I have also seen so many people with masks under their chins and they pull it up when they see a police officer.”
Through the office of community engagement meant to ensure that information about Covid-19 is communicated in a language the community best understands, the Ministry of Health says they have communicated the public health measures, like hand washing, wearing of masks, and maintaining physical distance to at least 12 million households in the country, especially those in slums, refugees and people living in arid and semi-arid areas.
According to the ministry, surveys show that people are changing their behaviour. But, Dr Bahizire said more still needed to be done for the public to take responsibility.
Just like in Ebola, Covid-19 requires that high standards of hygiene, especially handwashing, are maintained. It sounds simple, but there are all sorts of considerations: reminding people to use paper towels rather than material ones, ensuring that the taps can be turned off using an elbow rather than hands as well as proper usage of face masks. And in both cases, if you have symptoms, you must isolate.
Finally, people must own the disease. People want to relate to real people. It is, therefore, imperative for patients who have suffered from the disease to speak up.
“The first cases that come out and speak up will inspire people to own the disease. It will also reduce stigma. Because for now, when asked, many people will say they do not know anyone with Covid-19. The risk of this is that they think this disease is for others, unfortunately, some people may even think the numbers are made up,” says Dr Bahizire.



