Kenya to get doses of drug that shortens Covid-19 recovery time
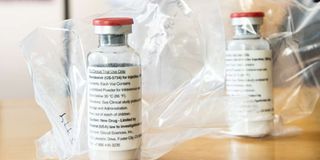
This file photograph taken on April 8, 2020, shows vials of the drug 'remdesivir' during a press conference on Covid-19 medication at The University Hospital Eppendorf (UKE) in Hamburg, northern Germany.
What you need to know:
- Remdesivir is in high demand after the intravenously-administered medicine helped to shorten hospital recovery times in a clinical trial.
- Because it is given intravenously over at least a five-day period, it is generally being used on patients sick enough to require hospitalisation.
Kenya is poised to receive an injectable new drug (remdesivir) found to shorten the recovery time of some hospitalised Covid-19 patients.
Remdesivir, an antiviral medication developed to treat Ebola that was in May approved for emergency use on Covid-19 patients, is one of the two drugs proven to work against Covid-19. The other one is dexamethasone.
Remdesivir is in high demand after the intravenously-administered medicine helped to shorten hospital recovery times in a clinical trial.
It is believed to be most effective in treating Covid-19 patients earlier in the course of disease than other therapies like the steroid dexamethasone.
Still, because it is given intravenously over at least a five-day period, it is generally being used on patients sick enough to require hospitalisation.
Kenya has been listed among 126 others identified by Gilead Sciences as low-income and lower-middle-income countries set to benefit from generic versions of the drug that will be manufactured by five companies licensed to produce it for developing countries.
EU GREENLIGHT
The European Commission Friday announced it had given conditional approval for the use of remdesivir in severe Covid-19 patients following an accelerated review process, making it the region’s first authorised therapy to treat the virus.
The EU’s green light to obtain doses for the 27 European Union countries expanded the global use of the drug after the US cleared it for emergency use and it is also approved as a Covid-19 therapy in Japan, Taiwan, India, Singapore, and the United Arab Emirates.
Remdesivir, which was trialled in the Ebola epidemic but failed to work as expected, is under patent to Gilead, which means no other company in wealthy countries can make it.
However, through a non-exclusive voluntary licensing agreement with the pharmaceutical manufacturers located in India and Pakistan produce and sell the treatment “at a substantially lower cost,” the Gilead said.
The companies, Cipla Ltd., Ferozsons Laboratories, Hetero Labs Ltd., Jubilant Lifesciences and Mylan will manufacture the drug for distribution in “low-income and lower-middle-income countries, as well as several upper-middle- and high-income countries” that face health-care obstacles amid the coronavirus pandemic, the parent company, Gilead Science, posted on its website.
Gilead Sciences, an American biopharmaceutical company that researches, develops and commercialises drugs, is the maker of Remdesivir, the first covid-19 treatment found to have worked in clinical trials.
Under the licensing agreements, the companies have a right to receive a technology transfer of the Gilead manufacturing process to enable them to scale up production more quickly.
Generic drugs are copies of brand-name drugs that have exactly the same dosage, intended use, effects, side effects, route of administration, risks, safety, and strength as the original drug.
“The licenses are royalty-free until the World Health Organization declares the end of the Public Health Emergency of International Concern regarding Covid-19, or until a pharmaceutical product other than Remdesivir or a vaccine is approved to treat or prevent Covid-19, whichever is earlier,” Gilead says on its website.
CHARGES
Last week the Company announced that it will charge high-income countries’ governments for Sh41,676 ($390) a vial—for a total of Sh250,058 ($2,340) for standard six-day treatment (with a double dose on the first day).
In the US, however, the company set two separate prices. One, Sh41,676 ($390), is the same paid by all other wealthy countries, and the other, Sh55,593 ($520), charged to America’s private buyers, such as hospitals, which will spend Sh333,372 ($3,120) for the typical treatment.
“As with many aspects of this pandemic, we are in uncharted territory in pricing remdesivir,” Gilead’s chairman and chief executive, Daniel O’Day, wrote in an open letter Monday morning.
“As the world continues to reel from the human, social, and economic impact of this pandemic, we believe that pricing Remdesivir well below value is the right and responsible thing to do.”
However, for countries like Kenya, the five generic manufacturers will set their own prices for the generic product they produce.
US PURCHASE
Gilead invented the drug about 10 years ago when it was searching for treatments for hepatitis C but did not develop it.
Later, the drug’s potential as an antiviral for emerging diseases was explored through a partnership with the government. According to the vompany, it will have spent Sh107 billion ($1 billion) to develop and manufacture the drug by the end of 2020.
Soon after the announcement, the Trump administration said it had secured nearly all of the company’s supply of the drug for use in US hospitals through September, with a contract for 500,000 treatment courses, which it will make available to hospitals at Gilead’s price.
No other country will be able to buy remdesivir for the next three months at least.
The first 140,000 doses which were supplied to drug trials around the world have been used up making experts and campaigners worried by the US unilateral action and the wider implications.
This is especially because the US has so far shown it is prepared to outbid and outmanoeuvre all other countries to secure the medical supplies it needs as the country bought all of Gilead’s production for July and 90 per cent for August and September.





