Day in life of nurses looking after virus patients
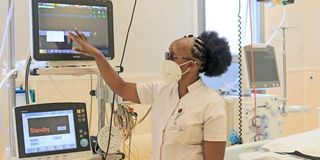
Wambui Njenga a senior Nurse at The Nairobi Hospital shows some of the equipment she uses in the Critical Care unit (CCU) to save lives of Covid-19 patients on July 3, 2020. PHOTO| SILA KIPLAGAT | NATION MEDIA GROUP
What you need to know:
- In a hospital full of a deadly, highly contagious viruses, they have to protect themselves with face masks, stoicism and prayer.
What does it take to take care of Covid-19 patients, more so the ones in intensive care units, who can barely talk and depend fully on healthcare workers?
As the new coronavirus cases surge, thousands of healthcare workers are risking their lives on the frontline, with Kenya Medical Practitioners, Pharmacists and Dentists Union acting secretary-general Chibanzi Mwachonda saying Saturday that two nurses have so far succumbed to Covid-19.
The revelation came two days after a gynaecologist, Dr Adisa Lugalika, died on Thursday of the virus.
Most health workers sometimes stay away from home for weeks to avoid infecting their family, with reports indicating 292 of the workers have been infected.
Our Health and Science reporter Angela Oketch spoke to four nurses, who spend more than 50 hours a week in the Covid-19 ICU, treating critically ill patients. They discuss the risks, the workload, moral challenges and the emotional toll it’s all taking on them.
JOYCE NJERI, ICU NURSE, KENYATTA UNIVERSITY TEACHING, REFERRAL AND RESEARCH HOSPITAL

Joyce Njeri.
Njeri spends at least two weeks away from her family every month due to her job, despite the fact that they live in the same county. She works for a week at the hospital then stays at the facility’s hostel for two weeks in quarantine.
She is then tested and her body monitored to ensure she did not contract coronavirus while attending to patients.
“When I am attending to patients, I am given a room at the hospital for a week since we work in shifts. Then I am off duty, I am tested, and I have to stay at the hospital for another week, when the test turns negative, I join my family,” she says.
She attends to her patients while we watch through a barricaded glass. She sings and talks to them, though very few can hear her voice. This brings her peace.
They lie unconsciously in their beds, having been pushed to the brink of death by the disease that has killed at least 154,000 people and affected 11 million others globally.
“They can still hear me,” says the critical care nurse at Kenyatta University, Teaching and Referral Hospital, adding that she is all the patients have since they do not allow family members to visit.
Two weeks ago, she lost one of the patients who was successfully taken off a ventilator and was put back after breathing problems recurred.
“He died in the night. He was brought when he could barely talk, he was breathless, the 84 year old man struggled and you could see that he was willing to do all within him to live, when he had just recovered. I was saddened, says Njeri.
She takes care of two critically ill patients in a day. Since the country reported the first case on March 13, she has attended to 50 patients in ICU who she considers part of her family.
They work in shift rotation with long days and nights of 13 hours each, up to seven days a week. This is done to provide consistency for patients and colleagues, but also to reduce the number of days we go in.
Emillie Ashihundu, ICU nurse, Aga Khan

Emillie Ashihundu, ICU nurse, Aga Khan.
Emillie Ashihundu’s mother is more worried than she is and keeps checking on her every morning before she leaves for work and every evening when she gets back to the house.
The mother of three, a critical care nurse and intensive care unit manager at Aga Khan Hospital, has had to assure her mother that all will be well.
“The best they can do is to pray for me. This is the job I chose and I am taking all the precautions to ensure that I do not put my colleagues at risk and my family as well,” she says.
She continues: “The fear is real but we have to be there for our patients,” says the soft-spoken Emillie who has to be there every morning to ensure that her junior staff are well-protected to get into the wards and attend to patients.
She has to be there when they are donning and doffing off their personal protective equipment to avoid any infection.
The anxiety that surrounds the pandemic is too loud.
“Every morning we get to know who is getting in the wards, then we put on the equipment together as a team, after which, we do a checklist to ensure that they are properly worn and protected to avoid any mistake,” she says.
The main challenge is always when doffing. “When you are putting on the equipment, you sweat too much, because one has to stay in the room for over three hours attending to the patients,” she says.
For the past four months, she has not had a social life to ease the steam. Her life revolves around her house and the hospital.
Irene Wahome, ICU manager, Kenyatta University Teaching and referral Hospital

Irene Wahome, ICU manager, Kenyatta University Teaching and referral Hospital.
Emotionally, Irene is very weak, more so when she loses a patient that she is attached to. However, she has to be strong for her staff since she is in charge of ensuring that they are stable both at work and at home.
“I get disturbed a lot. I would rather go back home and cry than do it at the hospital where they will be able to see me,” she says
She ensures that they get psychological support, they are fed well and their houses are fumigated after every shift.
“I do double work, checking on them when they are at work and at home because if any gets infected at home, it’s a risk to my staff. So it’s a double work. They also have to be tested when they are getting back to work and given vitamin C to boost their immunity.
In a hospital full of a deadly, highly contagious viruses, they have to protect themselves with face masks, stoicism and prayer.
“We pray together every morning as a team for God’s protection when we go to the battle,” she says.
Wambui Njenga, critical care nurse at the Nairobi Hospital

Wambui Njenga, critical care nurse at the Nairobi Hospital.
A feeling of powerlessness sank in when one of her colleagues was infected with the virus last month. This affected her for some time until she learnt that the colleague had recovered.
“For most of us this job is a vocation, so it’s shocking and frustrating to see those who attend to patients being attended to,” she said.
However, she still fears that she could get infected since she is attending to critically ill patients who literally depend on her to massage, feed, give medication and even bathe.
Every day, she struggles to protect her patients, her family and herself from getting the coronavirus by ensuring that she puts on the protective equipment correctly and removes them off under her colleagues’ watch.
“We all feel really burnt out and worried about the infection but I just want to see my patients getting out of their unconscious bed and walking to the general wards better than they came,” says Ms Njenga, a critical care nurse working at the Nairobi Hospital caring only for Covid-19 patients.
“At the end of the day, it has to be done. Somebody has to take care of these people,” she said. “There’s no time to be too concerned for ourselves. We take the proper precautions, and we do what we have to do for the patients.”
She feels guilty for not being there for her husband and child as it used to be in the past since she is not giving them much of their time but this is for their safety.
“I am taking precautions. I don’t want to put them at risk,” she says.
The one family-safety measure she agrees on and practises is extreme hygiene.
“She strips down as soon as possible she gets to her door, clothes straight to the laundry, she sprays off, her shoes, her job card with disinfectant, and then heads straight to the shower,” says the mother of one.
Wambui, plain-spoken, says her fate is in God’s hands.





