Tough questions for Kenya as Covid-19 spreads
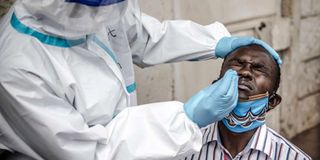
Coronavirus testing in Kawangware slums, Nairobi, on May 1, 2020. PHOTO | LUIS TATO | AFP
What you need to know:
- Apart from the immunity and institutional structures, Prof Kariuki says it helps that the population in Kenya is majorly young, with a median age of 20 years.
- Poverty among Kenya’s young has exposed their bodies to many elements and coached them to survive all manner of assaults.
Question: Where does Kenya stand on the coronavirus risk index? How many Kenyans are likely to be infected by the virus before it finally peters out?
Out of the infected, how many will require hospital care? How many will die? When?
The Sunday Nation has spent the past three weeks trying to answer these questions, talking to virologists, epidemiologists, mathematicians and all manner of experts.
It has attended numerous press conferences, shot tens of questions to Ministry of Health officials and studied tomes of research papers on the Covid-19 pandemic. In the end, we have come to an unfavourable conclusion: the number of infections, their peak, and cumulative deaths depend on who you ask. And the numbers are as varied as the projections.
This week a team of researchers at the University of Nairobi told the Senate that their worst-case-scenario modelling showed that about 620,000 Kenyans could die of the virus by February next year.
At about the same time, another team of researchers from Washington State University in the US noted that Kenya’s, and generally Africa’s, death toll from the virus could be much lower than the global average because of a number of environmental, immunological and demographic factors.
And those two studies, coming hot on the heels of each other, illustrate how hard it has become to plot the trajectory of Covid-19 in Kenya.
Thus, the answers to the questions at the start of this article are all similar and curt: it depends on who you ask.
ASYMPTOMATIC
In the worst-case-scenario model by the UoN, researchers note that about two million Kenyans will be asymptomatic and about 356,000 moderately affected by the virus, while 114,470 others will need crucial medical attention, including intensive care and ventilators.
Prof Omu Anzala, director of the Kenya Aids Vaccine Initiative, presented the findings to the Senate this week and noted that the model assumed uniform transmission across the country and prevalent asymptomatics.
The Ministry of Health has previously said that 90 per cent of Kenyans infected are asymptomatic. “Behaviour change will determine the change in the modelling,” said Prof Anzala.
The model, conducted by researchers at the University of Nairobi’s College of Health Sciences, estimates that the peak in health care utilisation will occur around February 2021, with up to 356,000 hospital beds and 115,000 ventilators required in that month to accommodate the high numbers.
But Prof Kariuki Njenga of the Washington State University and a senior research officer at the Kenya Medical Research Institute (Kemri), thinks that Kenya might not get to the predicted horrors.
In a paper scheduled for publication in the American Journal of Tropical Medicine, he argues that the “low seeding rate” of the virus – seeding rate refers to the number of initial contaminations from abroad – effective mitigation measures, a population that is more youthful, favourable weather and possible pre-existing immunity due to prior exposure to other coronaviruses” might be working in our favour.
ZOONOTIC
These factors, he notes, could explain why deaths in Africa are four-fold less than those in Europe and North America and two-fold less than those in Asia and South America.
However, it is the argument that “a population across Africa has some level of Sarc-CoV-2 immunity due to prior exposure to other coronaviruses” that lit up the bulb over our heads.
Was there merit in that assumption? Could it be scientifically proven? Could it explain the high cases – at 90 per cent – of asymptomatic infections in Kenya?
The CDC defines coronaviruses as a large family of viruses that cause respiratory illnesses and include the viruses that cause Sars and Mers, as well as those that cause milder illnesses, like the common cold.
These viruses are zoonotic, meaning they originate from animals, then come to people. So far seven of them have made this migration: four little-known ones that have been implicated in causing mild flu; the Middle East Respiratory Syndrome (Mers) and Severe Acute Respiratory Syndrome (Sars).
This spillover from animals to people has happened several times, and there is evidence that strains closely related to human coronaviruses are circulating within bat populations in Africa and elsewhere, notes Prof Kariuki while advancing the immunity argument.
DEVELOPING IMMUNITY
In April, Prof Anzala and a team of researchers from the University of Helsinki in Finland discovered a sixth Ebola virus species – Bombali ebolavirus – in an Angolan free-tailed bat in the Taita Hills region of Kenya.
Meanwhile, Prof Kariuki and medical epidemiologist Isaac Ngere have an ongoing study on the Mers-CoV and found widespread virus transmission in African dromedary camels, the natural reservoir of the virus and few acute human cases in Marsabit and the region.
But these do not cause Covid-19, so how did exposure to them help us develop immunity against Sarc-CoV-2, the virus that causes Covid-19?
To answer that question, we contacted Prof Thumbi Ndung’u, a professor of virology based at South Africa’s Nelson R Mandela School of Medicine at the University of KwaZulu-Natal, and whose lab is part of the response team for South Africa.
He explained that “all viruses look for a receptor, a protein on the cell surface that they can land on before they attack the body”, and that “when you make a vaccine, or when the body develops immunity, you target that receptor so that the disease-causing virus is not able to attach to the human cell”.
YOUNG POPULATION
Prof Kariuki’s paper marshalled studies that show similarities in the body’s response to coronaviruses and other viruses, such as Sarc-C0V-1, and haemorrhagic fevers, such as Ebola, Lassa and Marburg, and Dr Ahmed Ogwell, Deputy Director of Africa Centers for Disease Control and Prevention, told the Sunday Nation that Africa had battled these diseases and already had systems in place, which could have worked in its favour.
“Kenya and other African countries knew the severity of what they were about to face and responded really quickly because they learnt from Ebola and the others that if you delay, you will not catch up,” said Dr Ogwell.
Apart from the immunity and institutional structures, Prof Kariuki says it helps that the population in Kenya is majorly young, with a median age of 20 years.
Higher fatalities have been recorded in countries with many older people and median ages of between 38 and 45 years, as seen in Spain, Italy, the United Kingdom and the United States.
Dr Ogwell agrees with the age explanation in part. “It is not just young people, but young healthy people,” he says.
But it is also this agility that makes them “superspreaders” because they are often sick but do not show signs. That agility also makes it hard for them to be detected by surveillance systems.
POVERTY, WEATHER
Dr Ogwell introduces another dimension to the argument, arguing that poverty among Kenya’s young has exposed their bodies to many elements and coached them to survive all manner of assaults.
On May 24, Kenyan scientist Fredros Okumu, who is the Director of Science at Tanzania’s Ifakara Health Institute, adopted that line of argument when he tweeted: “Don't underestimate the immunity of people who’ve lived all their life in non-sanitised environments.”
The final factor in favour of Kenya, according to Prof Kariuki, it its weather. “Africa experiences warmer and drier weather in the December-to-April season, with average day temperatures greater than 20 degrees Celsius in the entire sub-Saharan region and more than 30 of the 46 countries of that region averaging greater than 25 degrees Celsius.”
He notes that “only countries in the northern region, including Tunisia, Algeria, Egypt, Libya and Morocco, have day temperatures at less than 20”, and that infections have been considerably higher there.
So where are we, and where are we heading? It depends on who you ask.





