All you need to know about emergency care in Kenya
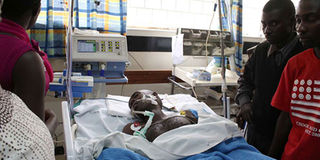
This photo taken on October 8, 2015 shows Alex Madaga admitted at Kenyatta National Hospital's intensive care unit. He later passed away. PHOTO | FILE | NATION MEDIA GROUP
What you need to know:
- The Ministry of Health in Kenya reported that in 2016, about 13,159 people were seriously injured on the road.
- The international Federation of Red Cross and Red Crescent Societies reports that more than half of deaths from road traffic accidents occur in the first few minutes after the crash.
The case of Alex Madaga, who died after waiting in the van for many hours after an accident, attracted uproar from all quarters.
He died in the “golden hour”, those few seconds where first aid such as stopping blood flow and preserving a blocked airway can buy an injured person enough time to reach the hospital alive.
This is the fate of more than 5,000 Kenyans every year who die in road accidents, due to a weak system of emergency medical care and referral.

This photo taken on October 8, 2015 shows Alex Madaga admitted at Kenyatta National Hospital's intensive care unit. He later passed away. PHOTO | FILE | NATION MEDIA GROUP
The Ministry of Health in Kenya reported that in 2016, about 13,159 people were seriously injured on the road.
The international Federation of Red Cross and Red Crescent Societies reports that more than half of deaths from road traffic accidents occur in the first few minutes after the crash.
JUST A FEW MINUTES
In a commentary at The Guardian, Red Cross Africa Director Alasan Senghore wrote that it can take just four minutes for a blocked airway to be fatal as it takes much longer than this for emergency services to arrive.
It is not just road traffic accidents, but also tens of thousands others lose their lives due to other emergencies such as heart attacks, stroke, maternity cases such as the killer pregnancy-induced blood pressure and falls from buildings.
Dr Benjamin Wachira, Kenya’s only licensed medical emergency expert, told Nation Life&Style: “At any point, every one of us will need emergency care. Any of us will develop an acute sickness that needs a medic’s attention quick…a fall, high blood pressure in pregnancy, labour and many others”.
He described the situation in Kenya: “Here people get a heart attack, stroke or any other medical problem that can be sorted out, but die because they were not able to get to a doctor fast enough.”
Those that make it to the hospital, through good Samaritans, are handled improperly that they end up dying in resuscitating tables in the emergency department, disabled for life or spend months in the hospital.
Mishandled or not, more than 80 per cent of the critical and bearable cases land at the Kenyatta National Hospital’s Accidents and Emergency department (A&E).
On any given day, KNH handles about 300 patients at the small department that acts the door to the hospital.

Kenyatta National Hospital. FILE PHOTO | NATION MEDIA GROUP
Like in any other facility, A and E is the most important part of the patients care because you do not go to any part of the hospital before passing through here.
YANKED FROM THE JAWS OF DEATH
It is here where patients are yanked from the jaws of death first before specialists can conduct surgeries or run tests.
According to the facility’s statistics unit, the accidents and emergency unit handled 105,134 patients in 2016 alone, which comprised both accidents and other emergencies.
In a day they are about 300, a figure that is hardly newsworthy for Kenya’s and the region’s largest hospital.
Nearly 72 per cent of these (75, 717) were new admissions while the rest (29,417) were old cases.
Nation Life&Style: spent time in the department for four days in 2017, a visit that proved that it is at the emergency room where all that is wrong with Kenya’s health system is seen.
The patients being wheeled into the unit are sometimes pieces of bones and flesh falling off the stretchers.
The crowd throngs the entrance of the room and a nurse barks orders to get some of the relatives of patients to get out.
Just like in the scene of accidents, these people block the movement of hospital staff here.
The head of the department Dr Alice Maingi, is particularly uneasy about seeing children in this floor as she says they could pick the worst pathogens here.
In the background, a patient complains that she has not been attended to for hours.
The nurses are not perturbed by that complaint because there is a queue and protocol that has to be followed: to attend to the most critical cases first
‘A GREEN’
Dr Maingi says “that is a green”. A green is a patient who can wait up to four hours, their lives are not hanging on a thread.
In a minute, the calm is interrupted. A seven-year-old child had fallen down to a concrete floor from four floors, and was rushed here a private car—fatal mistake number one, Dr Maingi said.
“In an ambulance there would have been equipment to keep her alive until she got here”, Dr Maingi said. But that is hardly surprising.
Dr Wachira and his colleagues conducted a study which showed that the public and the police don’t have the most basic first aid, let alone an accident where injuries that are traumatic, medical and obstetric in nature are experienced.
This baby was lucky to get a car but she had been a “red”— those for whom a second could mean they die— after sustaining severe multiple fractures from that fall, and was quickly rushed to resuscitation room A.
CASE NOT ISOLATED
Resuscitation room A is for people who need second-to-second life support and monitoring. Coming out of that room alive is a miracle, and those who do, spend a whole lot of time recovering. Dr Maingi is concerned about the paediatric cases of falls that the department she has been receiving.
This child’s trauma not isolated.
“They are too many, and the children die horrendous deaths either in the many construction sites that go on, grills through which they can slip… I do not know,” she says, trailing off.
Of the 1,639 that are rushed here after falling, more than half had been children, some are toddlers, just learning to walk.
The rest are young men, who get into bar fights, are lynched by the mob or fall off motorbikes. Most of the young men sustain brain injuries— very different from just a head injury— which is almost a sure death sentence.
Then there is an “Orange”. The “orange” patients have to be monitored so closely because in one second they could become “a red”, and at red, they die in less than ten seconds.
NO CURRICULUM
Even with the goodwill of most of the healthcare workers, there‘s no curriculum for training emergency medicine in Kenya.
Africa needs emergency care specialists. The World Health Organisation reports that 700 people die on the road every day in Africa. This 250 per cent higher than in Europe yet the continent owns 10 per cent of global motor vehicles.
In 2018, the Aga Khan Hospital, in partnership with Emergency Medicine Kenya Foundation launched their postgraduate training on the course, allowing doctors to come for a year and a half for a diploma.
When Dr Peter Halestrap from Kijabe Hospital looked at the deaths in the A&E, he decided to run a diploma course for clinical officers.
To his shock the deaths reduced by 50 per cent in the first few months. Aga Khan hospital also offers this course.
Dr Wachira, who got his postgraduate in South Africa, said that most of the hospital’s emergency centres in Kenya are run by medical and clinical officers who are ill-equipped to handle the rush that is needed to save a life before they can be seen by a clinician.
This damns Kenya’s referral system to be categorised as “underdeveloped”— there is “mature” and “developing” such as South Africa’s where Dr Wachira trained.
AMBULANCES COSTLY
The cost of ambulances that are specifically manufactured for this care are expensive; and the Kenya Bureau of Standards has since halted the purchase of vans for them to be turned into ambulances.

Ambulances rushing injured people to a hospital in a past photo. PHOTO | WILLIAM OERI | NATION MEDIA GROUP
Recalling his training in South Africa, Dr Wachira said “I had a patient who was stabbed with a knife to the heart, he was rushed to the emergency department in four minutes, I stabilise him and in a few minutes the surgeon would take over and the following day I was saying hallo to that person as he invited me for coffee once he was discharged.
Dr Wachira, who now heads the emergency unit at the Aga Khan, added “I always wondered why I never saw these cases in Kenya, it was because in Kenya, you get stabbed like that, you die, you do not even make it here”.
There is some truth to that because KNH had 503 “rotting deads”, a term in the emergency room to mean patients who were brought when they were dead already.
LESSONS, FROM SOUTH AFRICA AND GHANA
In the municipal of Gauteng in South Africa, the community has partnered with the university of Johannesburg’s college of health sciences, a technology company Philips so that the process of evacuation from the home, to transportation and to the hospital are smooth.
Nation Life&Style observed how pregnant women who were the biggest casualties in the modest neighbourhood had their lives saved in the care of community health volunteers who knew how to call the ambulances, which had trained paramedics with equipment that monitored vitals of both the baby and the mother automatically.
The Dean of Faculty of Health sciences Prof Andre Swart told Nation Life&Style in a 2015 visit that the equipment allowed the paramedics to concentrate on stabilising the mother, knowing when to inject or not as well as communicate the information of the patient they were ferrying to the hospital.
In Ghana, nearly 90,000 drivers have been trained on how to respond to injuries in road traffic accidents.
The world Health Organisation reports that over 16,000 die or are injured annually in Ghana in roads
In Uganda where 151 in every 10,000 people die in Road accidents every year, more than 2,000 drivers and teachers have been trained and first aid spots located in danger zones near the country.





