WHO: One in 10 of medical products in low and middle-income countries are fake
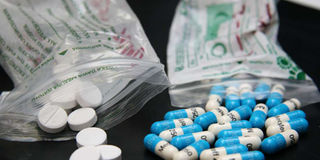
Fake medicine bought at a hospital on August 24, 2013. One in every 10 medical products circulating in low and middle-income countries were either substandard or fake, according to a new research by the World Health Organization. PHOTO | FILE | NATION MEDIA GROUP
What you need to know:
- Since 2013, WHO has received 1,500 reports of cases of substandard or falsified products.
- The London School of Hygiene and Tropical Medicine estimates that 116,000 (64,000–158,000) additional deaths from malaria could be caused every year by fake antimalarial drugs in sub-Saharan Africa.
One in every 10 medical products circulating in low and middle-income countries were either substandard or fake, according to a new research by the World Health Organization.
This means that people were taking medicines that failed to treat or prevent disease.
SIDE EFFECTS
Not only is this a waste of money for individuals and health systems that purchase these products, but substandard or falsified medical products can cause serious illness or even death.
The findings were supported by Dr Walter Otieno, Western- Kenya based paediatrician who raised concern that most of his patients were complaining of reoccurrence of diseases.
“I have been in this field for long but the trend we are watching now is worrying. It’s either you send your patients to a renowned pharmacy or they would be treating one disease forever,” said Dr Otieno.
PHARMACY
He said he has had to deal with parents bringing their children to his clinic for a consecutive month until he has to change where they buy their medicine from.
“Pharmacy business has become lucrative that everyone wants to get into without considering where they will get the drugs; we are trading with people’s life. Taking poor drugs can be very dangerous,” he said.
Based on 10 per cent estimates of substandard and fake medicines, a modelling exercise developed by the University of Edinburgh estimates that 72,000 to 169,000 children may be dying each year from pneumonia due to substandard and falsified antibiotics.
FAKE DRUGS
A second model done by the London School of Hygiene and Tropical Medicine estimates that 116,000 (64,000–158,000) additional deaths from malaria could be caused every year by fake antimalarial drugs in sub-Saharan Africa, with a cost of $38.5 million (21.4 million–52.4 million) to patients and health providers for further care due to failure of treatment.
“Substandard medicines particularly affect the most vulnerable communities,” says Dr Tedros Adhanom Ghebreyesus, WHO Director-General.
“Imagine a mother who gives up food or other basic needs to pay for her child’s treatment, unaware that the medicines are substandard or falsified, and then that treatment causes her child to die. This is unacceptable. Countries have agreed on measures at the global level – it is time to translate them into tangible action,” he said.
TRAFFICKING
A UN study dated May ranked Mombasa as a major hub for trafficking of fake pharmaceutical and veterinary drugs, putting millions of lives in danger.
The study by the World Customs Organisation (WCO) and the International Institute for Research Against Counterfeit Medicines (IRACM) cites the Kenyan port city as being among the biggest trafficking points in Africa for counterfeit veterinary products and human medicines like antimalarials, anti-cancer, anti-inflammatories, antibiotics and analgesics as well as gastro-intestinal.
“Some 113 million illicit and potentially dangerous medicines were seized in Africa, with a total estimated value of €52 million (Sh6 billion).
The biggest interceptions were in Nigeria, Benin, Kenya and Togo in that order,” says WCO Secretary-General Kunio Mikuriya in the report.
COUNTERFEITS
The report, which covered 16 WCO member-states in Africa, shows that out of the new record seizure of 113 million illicit and potentially dangerous pharmaceutical products, more than 12 million (12,509,823) units were netted at the Mombasa seaport alone.
World Health Organization reports show that 700,000 people are killed globally by counterfeit medicines annually. Africa contributes 100,000 of these deaths.
Counterfeit (or illicit) medicines are drugs that are not allowed into the country either due to infringement of international property rights, licences, false certificates, transport or storage conditions, or those not declared.
They may also have wrong ingredient size or no active ingredients at all to cure illnesses.
VITAL
Since 2013, WHO has received 1,500 reports of cases of substandard or falsified products and of these antimalarials and antibiotics are the most commonly reported.
Most of the reports 42 per cent come from the WHO African Region, 21 per cent from the WHO Region of the Americas, and 21 per cent from the WHO European Region.
“Many of these products, like antibiotics, are vital for people’s survival and wellbeing,” says Dr Mariângela Simão, Assistant Director-General for Access to Medicines, Vaccines and Pharmaceuticals at WHO.
“Fake medicines not only have a tragic impact on individual patients and their families but also are a threat to antimicrobial resistance, adding to the worrying trend of medicines losing their power to treat”.
RESEARCH
This study was based on more than 100 published research papers on medicine quality surveys done in 88 low- and middle-income countries involving 48,000 samples of medicines.
Lack of accurate data means that these estimates are just an indication of the scale of the problem. More research is needed to more accurately estimate the threat posed by substandard and falsified medical products.
“Substandard medical products reach patients when the tools and technical capacity to enforce quality standards in manufacturing, supply and distribution are limited. Falsified products, on the other hand, tend to circulate where inadequate regulation and governance are compounded by unethical practice by wholesalers, distributors, retailers and healthcare workers,” said Dr Simão.
He said more research is needed to determine the proportion and impact of sales of substandard or falsified medical products.
“The bottom line is that this is a global problem,” says Dr Simão. “Countries need to assess the extent of the problem at home and cooperate regionally and globally to prevent the traffic of these products and improve detection and response.”





