Report lays bare Kenya's frail health sector
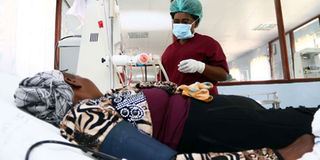
A doctor attends to a patient at Nakuru Level Five Hospital on March 15, 2017. Specialists constituted 37 per cent of the number of active and retained medics in 2015. PHOTO | SULEIMAN MBATIAH | NATION MEDIA GROUP
What you need to know:
- Kenya is still far from the WHO recommended ratio of 44.5 nurses, physicians and doctors to take care of 10,000 people.
- The report also exposed inequalities in the distribution of health workers in the various counties.
Kenya has only 2,089 specialist doctors, a new national survey of the country’s hospital staff has revealed.
In 2015, there were 5,660 medical doctors, with 387 of them specialising in gynaecology.
Experts in general surgery stood at 338 while internal medicine experts were 296.
NON-COMMUNICABLE DISEASES
The 2015 Kenya Health Workforce Report: The Status of Health Care Professionals in Kenya, prepared by the Ministry of Health and America's Emory University, was released on Thursday last week.
It gathered data from more than 10 regulatory bodies between 2006 and 2015.
Specialists constituted 37 per cent of the number of active and retained medics in 2015.
The document lays bare Kenya’s ill-preparedness in tackling non-communicable diseases in terms of human resource capacity.
For instance, cancer killed about 15,714 people in 2015, according to the Ministry of Health, yet there are only nine experts in radiotherapy/oncology and 128 in radiology.
TRAINING INSTITUTIONS
There are only 71 psychiatrists in Kenya yet the latest global report on mental health by the World Health Organization (WHO) showed that about 4.4 per cent of Kenyans – over 2 million people – have a mental problem of some sort.
For all the cases of diabetes, there is only one diabetologist.
The report noted the growth in the number of healthcare workers in Kenya in that period of time, mainly attributed to the increase in training institutions.
There were only two medical schools in Kenya in 2006, now there are 10 as nursing schools increased from 77 to 102 during the same period.
Despite this positive trajectory, Kenya is still far from the WHO recommended ratio of 44.5 nurses, physicians and doctors for 10,000 people.
POPULATION GROWTH
Kenya is at a distant 13.8 per 10,000. The report calculated that the total population was 47,681,799 people in January 2016, and that on a given day there are 4,373 live births and 1,164 deaths.
Therefore, Kenya's population grows by more than 3,200 every day but that does not match the rate at which new doctors are added to the market annually.
For the newborns, there were only 295 paediatricians and for the deaths, there were only 78 pathologists.
Other health workers fill this gap. After further training, clinical officers also become specialists.
Of the 10,562 active clinical officers by December 2015, 1,016 (9.6 per cent) had some type of special training with majority (292) in anaesthesia followed by paediatrics (255), otolaryngologists (ear, nose and throat specialists) 118, and lung and skin (110).
INEQUALITIES
This report also brought to fore the inequalities in the distribution of other health care workers in rich and poorer counties.
Nairobi had more than 28 health training institutions, with Kiambu and Kisumu with 14 and 11, respectively.
There was a direct link between the low number of health care workers to the training schools and internship centres in the counties.
The report also exposed inequalities in the distribution of health workers in the various counties with Nairobi holding more than 50 per cent of health workers.
The nurses’ national ratio per 10,000 is 8.3 but Nairobi had more standing at 9.7 nurses per 10,000 people as Uasin Gishu(8.5), Tharaka-Nithi (7.9), Isiolo (5.2), and Taita-Taveta (5) fared well.
DOCTOR TO PATIENT RATIO
Mandera, Wajir, Tana River, Nandi, Samburu, Narok, Turkana and Busia had less than one caregiver per 10,000.
When the specialist and general practitioner doctors are combined, the national ratio for doctors is 1.5 medics per 10,000 people while that of dentists is 0.2 dentists per 10,000.
Nairobi is still ahead of the pack with 9.5 doctors and 1.1 dentists per 10,000, followed by Mombasa (2.8), Uasin Gishu (2.1), Kisumu (1.6), Nyeri (1.3), Kiambu (1.1), and Isiolo (1.1).
All the other 40 counties have a ratio of less than 1 medic.
The national ratio of clinicians is 2.7 per 10,000 but five counties had a high ratio of clinical officers aged below 60 years, namely, Nyeri (7.3), Kisii (6.9), Baringo (6.7), Elgeyo Marakwet (5.2), and Busia (4.4).





