Mysterious infection spanning the globe in a climate of secrecy
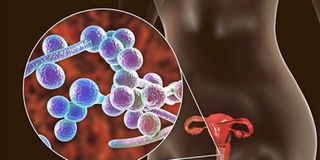
The germ, a fungus called Candida auris, preys on people with weakened immune systems, and it is quietly spreading across the globe. PHOTO | FOTOSEARCH
What you need to know:
- The germ, a fungus called Candida auris, preys on people with weakened immune systems, and it is quietly spreading across the globe.
- Scientists say that unless more effective new medicines are developed and unnecessary use of antimicrobial drugs is sharply curbed, risk will spread to healthier populations.
Last May, an elderly man was admitted to the Brooklyn branch of Mount Sinai Hospital for abdominal surgery. A blood test revealed that he was infected with a newly discovered germ as deadly as it was mysterious. Doctors swiftly isolated him in the intensive care unit.
The germ, a fungus called Candida auris, preys on people with weakened immune systems, and it is quietly spreading across the globe.
Over the last five years, it has hit a neonatal unit in Venezuela, swept through a hospital in Spain, forced a prestigious British medical centre to shut down its intensive care unit, and taken root in India, Pakistan and South Africa.
CLEANING
Recently C. auris reached New York, New Jersey and Illinois, leading the federal Centers for Disease Control and Prevention to add it to a list of germs deemed “urgent threats.”
The man at Mount Sinai died after 90 days in the hospital, but C. auris did not. Tests showed it was everywhere in his room, so invasive that the hospital needed special cleaning equipment and had to rip out some of the ceiling and floor tiles to eradicate it.
“Everything was positive — the walls, the bed, the doors, the curtains, the phones, the sink, the whiteboard, the poles, the pump,” said Dr Scott Lorin, the hospital’s president.
INFECTIONS
C. auris is so tenacious, in part, because it is impervious to major anti-fungal medications, making it a new example of one of the world’s most intractable health threats: the rise of drug-resistant infections.
For decades, public health experts have warned that the overuse of antibiotics was reducing the effectiveness of drugs that have lengthened lifespans by curing bacterial infections once commonly fatal.
But lately, there has been an explosion of resistant fungi as well, adding a new and frightening dimension to a phenomenon that is undermining a pillar of modern medicine.
“It’s an enormous problem,” said Matthew Fisher, a professor of fungal epidemiology at Imperial College London, who was a co-author of a recent scientific review on the rise of resistant fungi. “We depend on being able to treat those patients with anti-fungals.” Simply put, fungi, just like bacteria, are evolving defences to survive modern medicines.
RESISTANT
Yet even as world health leaders have pleaded for more restraint in prescribing antimicrobial drugs to combat bacteria and fungi — convening the United Nations General Assembly in 2016 to manage an emerging crisis — gluttonous overuse of them in hospitals, clinics and farming has continued.
Resistant germs are often called “superbugs,” but this is simplistic because they don’t typically kill everyone. Instead, they are most lethal to people with immature or compromised immune systems, including newborns and the elderly, smokers, diabetics and people with autoimmune disorders who take steroids that suppress the body’s defences.
CANCER
Scientists say that unless more effective new medicines are developed and unnecessary use of antimicrobial drugs is sharply curbed, risk will spread to healthier populations.
A study the British government funded projects that if policies are not put in place to slow the rise of drug resistance, 10 million people could die worldwide of all such infections in 2050, eclipsing the eight million expected to die that year from cancer.
In the US, two million people contract resistant infections annually, and 23,000 die from them, according to the official CDC estimate.





