Have girls vaccinated against cervical cancer
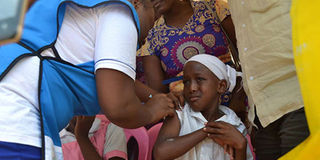
An eight-year-old girl receives the cervical cancer vaccine at Hola Referral Hospital, in Tana River County, on October 25, 2019. We may not have a say over other cancers, but let all our girls get this life-saving jab. PHOTO | STEPHEN ODUOR | NATION MEDIA GROUP
What you need to know:
- The slow and covert development of the disease fans its destructive effects, which come to the fore when it is too late for treatment to yield much.
- The vaccine is being used globally. Research has shown that it is safe and effective in protecting the recipient against diseases caused by HPV.
Last year, cancer become the second-leading cause of death, claiming 9.6 million lives — the reason any blow targeted at the scourge should be supported.
The World Health Organisation says 70 per cent of cancer deaths occur in low-income countries, such as Kenya — which is among those that have launched countrywide vaccination against Human Papilloma Virus (HPV).
HPV and Hepatitis infections, though preventable through vaccination, are responsible for 25 per cent of cancer cases in low- and middle-income countries.
The efforts by the Ministry of Health, international organisations and the support from the highest office on the land towards this initiative should be acknowledged by all.
We must work in synergy towards practical adoption by going for the vaccination and mobilising all girls of age 10 and above to get this life-saving jab.
ENCOURAGE UPTAKE
One of the reasons given by health communication experts for low uptake of medical interventions is the low-risk perception index of the lay public towards the disease or intervention in question.
Every human behaviour needs a trigger with a requisite threshold to result in a positive action.
To enhance uptake of such innovations, our health professionals need to lower themselves to the level of would-be recipients and give answers to these questions: what is HPV? Why should we be concerned? What are the benefits of the vaccine and punishment for not having it?
If these questions aren’t answered, then a man in my Lung’anyiro village will not see the reason to take his daughter for the vaccine; neither will the girl see the reason to endure the pain.
It gets murky where sexual behaviour is involved — as is the cause of some HPV infections.
The viral infection of the skin and mucous membranes, which is caused by a large variety of human papillomavirus, is spread through skin contact and vaginal, anal or oral sexual intercourse with an infected person.
PREVENTION
The slow and covert development of the disease fans its destructive effects, which come to the fore when it is too late for treatment to yield much.
HPV can remain silent for up to 20 years while the infected person spreads it unknowingly. Some HPV infections cause warts on the skin, vulva and around the anus, while some remain silent or cause cancers.
HPV is implicated in cervical cancer, which kills hundreds of thousands of women yearly. Cancers of the anus, penis, vagina, vulva and throat have been linked to HPV infection.
Before the vaccine, the virus was purely at the mercy of the body’s immune system to fight it off.
The vaccine is, therefore, a timely saviour whose single shot protects us from a myriad types of cancer.
MYTHS
And it only works when someone isn’t already infected with HPV, and it responds better in younger ages and can prevent most cases of cervical cancer.
The vaccine is being used globally. Research has shown that it is safe and effective in protecting the recipient against diseases caused by HPV.
Like any medical innovation, there are many myths around the vaccine — like its linkage to infertility and early sexual behaviour. All these have been proved wrong through research.
The saying that prevention is better than cure cannot find a better situation than one we are in. We may not have a say over other cancers, but let all our girls get this life-saving jab.
Dr Othieno is a veterinarian. [email protected]




